Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
This article if the first #Clinic_All project. It’s the result of team working on Twitter to develop something useful for clinicians in practice. Please follow all these wonderful people that have helped!..@DerekGriffin86 @PdKirwan @Seth0Neill @DrPeteMalliaras @DrAiLynTan @PhysioJack @Peter_Gettings @function2fitnes @AngeloCacchio and @unitedphysio. Apologies if I’ve missed anyone!
It’s also included online resources from rheumatology.org.uk, spondylitis.org and Medscape which have all been a great help. This is very much an ‘evolving piece’ my hope is it will be updated alongside emerging evidence. If you’d like to see how Twitter was used for this project see hashtags #TendonQ and #Clinic_All.
Thanks to everyone for their input so far!!
Management of tendinopathy has made great progress in recent years. Advances in research have improved our treatment options and our understanding of pathology. Despite this there are many who don’t respond well to current treatments and struggle with ongoing symptoms. This piece and its accompanying questionnaire (TendonQ) are to help clinicians identify other conditions that may be driving the tendinopathy and/ or slowing the progress made with rehab. It highlights how a thorough biopsychosocial approach is needed, especially in more complex cases.
First up is screening for rheumatological conditions that can cause tendon pain…I highly recommend listening to this great Physio Matters Podcast with @PhysioJack and @KarlGaffney1 – it works really well with this first section!…
When we think of tendinopathy we frequently think of a tendon responding to excess load, indeed this is often the classic history but other drivers need to be ruled out too. Tendinopathy can be a feature of rheumatological disease such as Spondyloarthropathy (e.g. Psoriatic Arthritis and Ankylosing Spondylitis) Rheumatoid Arthritis (RA) and Gout (Scott et al. 2015). Such conditions usually present with systemic symptoms including early morning stiffness, joint pain and swelling.
Source: Scott et al. (2015)
Spondyloarthropathies can be divided into 2 subgroups based on predominant symptoms; axial (affecting the spine) and peripheral (affecting the limbs) although there may be some overlap. They are associated with co-morbities both extra-articular (GEMS – Gut, Eyes, Mucosa, Skin) and peri-articular (enthesitis – insertional tendinopathy, plantar fasciitis);
Presentation of peripheral spondyloarthropathy can vary considerably from asymmetric, with only a few joints involved (pauciarticular) to predominant DIP joint involvement (typically associated with nail changes in Psoriatic Arthritis – see image below) to polyarticular symmetric arthritis which may appear similar to RA.
Axial spondyloarthropathy may also vary in severity and presentation. Several key features have been identified that help clinicians identify inflammatory back pain;
- Pain around the lower back, SIJ and buttock area. Alternating buttock pain.
- Eased by exercise, aggravated by prolonged inactivity
- Insidious onset
- Young age at onset (typically under 45 years old)
- Early morning stiffness lasting more than 30 minutes
- Night pain (usually in the second half of the night)
- At least 3 month duration
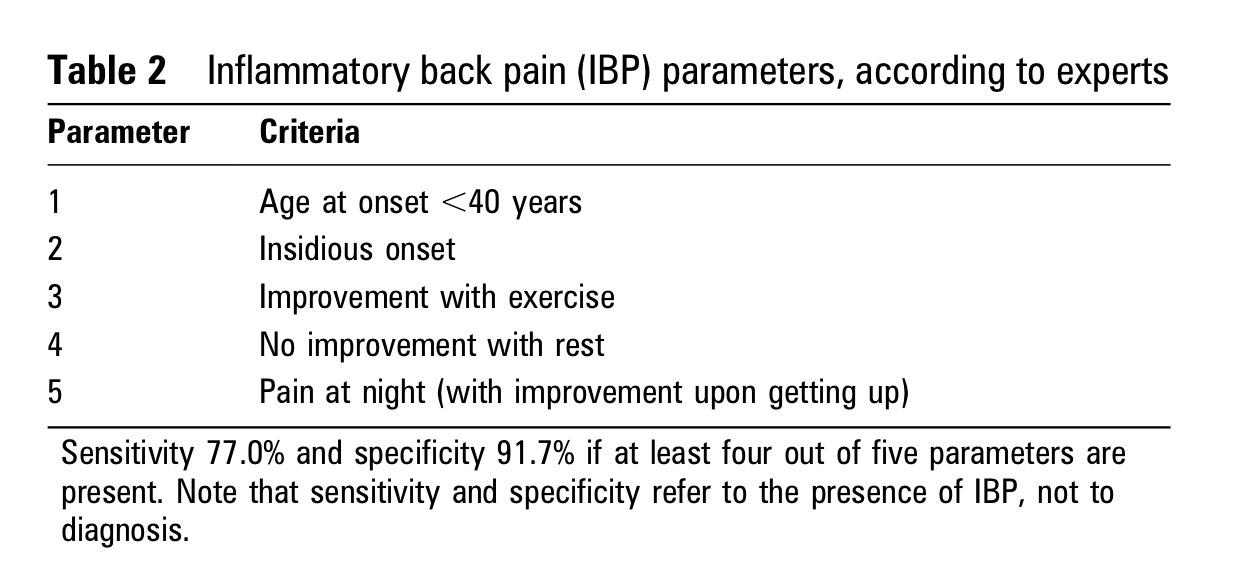
Sieper et al. (2009) suggested 5 parameters for identifying the presence of inflammatory back pain according to experts in the field;
……
Ankylosing Spondylitis
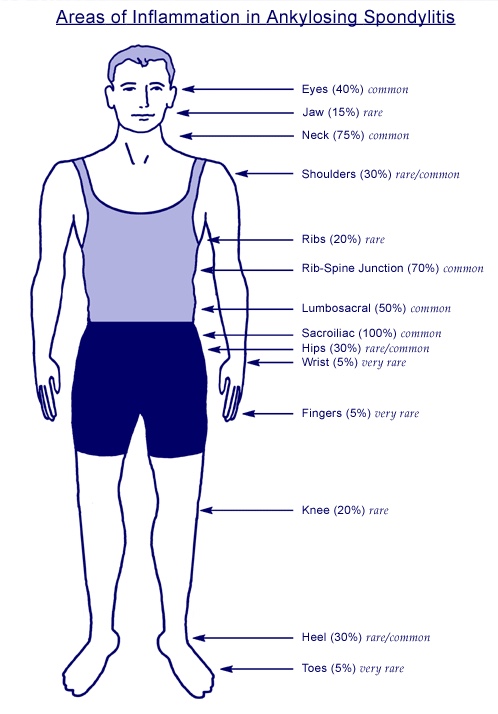
Ankylosing Spondylitis (AS) typically presents with axial symptoms as discussed above but can include multiple symptomatic areas;
Source: Spondylitis.org
The Irish Society for Rheumatology developed this AS screen form which can be useful for suspected AS.
Psoriatic Arthritis (PsA)
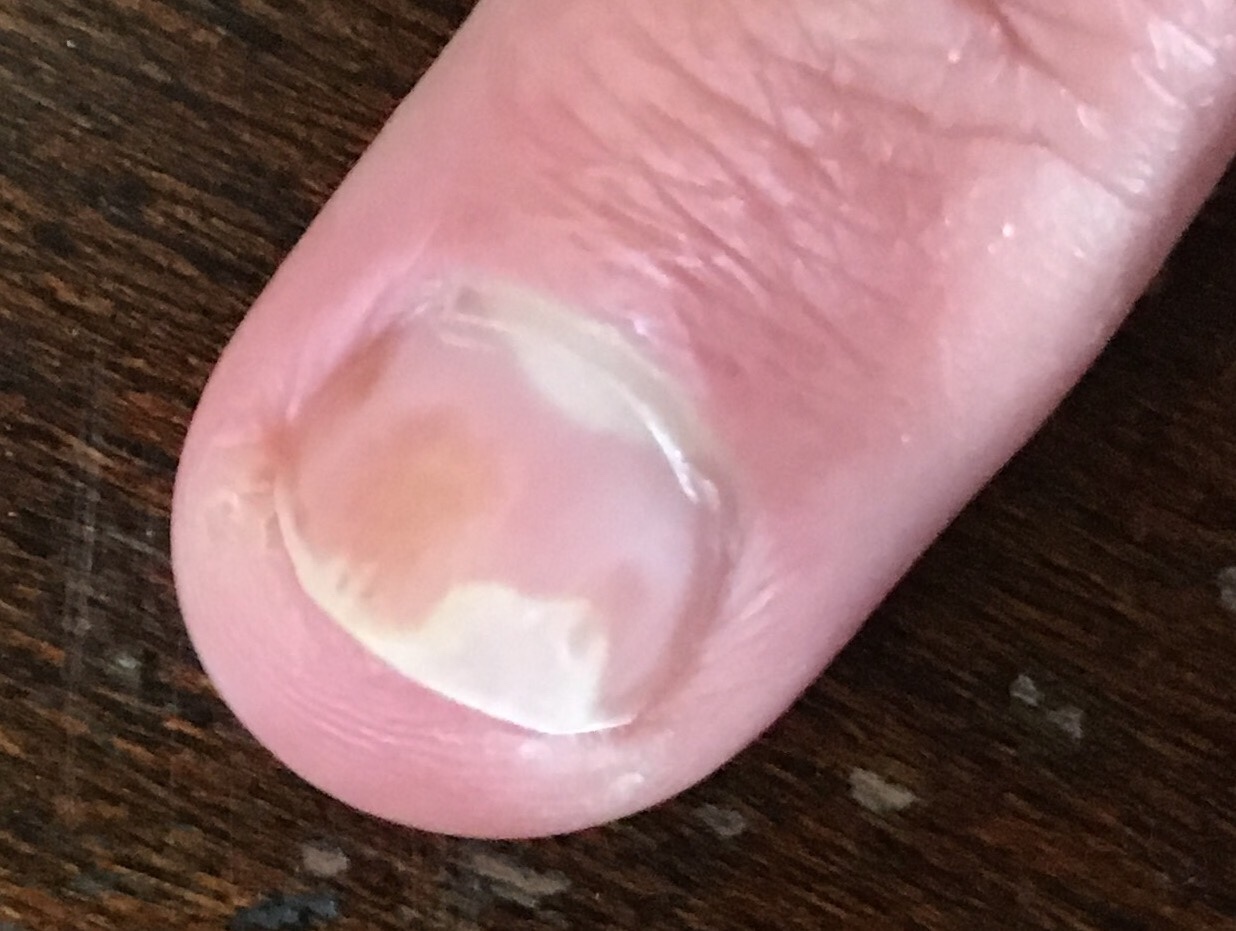
Psoriatic Arthritis (PsA) is a spondyolarthropathy usually linked to the skin condition psoriasis which typically presents as red, flaky patches of skin. The Psoriasis Foundation suggests that around 30% of those with psoriasis will go on to develop PsA. Those with nail changes (see below) are more likely to develop inflammatory joint symptoms so if you identify thickening, whitening or pitting of the nails it should raise your index of suspicion. The British Association of Dermatologists developed this assessment form for suspected PsA. I have a history of psoriasis, nail changes, joint pain (albeit very mild) and proximal hamstring tendinopathy which has prompted me to see a rheumalogist (more on that here).
Rheumatoid Arthritis
Rheumatoid Arthritis (RA) is a separate disease entity from the spondyloarthropathies. It’s characterised by symmetrical polyarticular joint inflammation, commonly affecting the metacarpophalangeal, proximal interphalangeal and metatarsophalangeal joints as well as the wrist and knees. Morning stiffness in and around the joint lasting at least an hour is a typical sign of RA (Grassi et al. 1998). Extra-articular features can include fatigue, feveret (slight fever), weight loss and malaise. RA can have significant effects on the tendon and tendon sheath. Tendinopathy of the wrist extensors is common and can lead to rupture (McQueen et al. 2005).
A further consideration with RA is what medication a patient may take. Some may have been on long term steroids which will influence the tendon as discussed in the medication section below.
Gout
Top physio and Clinical Research Fellow Paul Kirwan (@PDKirwan) kindly shared his expertise on gout,
“Gout is a crystal arthropathy, now that is not a very easy condition to understand, so I use this example, which was given to me by a Rheumatology consultant I work with.
Think of it similarly to a cup of tea with sugar being put in it, sugar is a crystal, and as you put sugar in to the cup of tea, the sugar dissolves in the tea, but if you keep adding sugar to the tea, eventually you will get to a point where no more sugar can be dissolved in the tea, the tea is supersaturated, and the sugar crystals deposit at the bottom of the cup.
Well gout is a little like this, but instead of sugar as the crystal, we have uric acid or urate as the crystal. We all have uric acid circulating in our blood stream, but if the levels of uric acid rise above the normal level, then there is a point where there is too much uric acid to stay in solution (ie: in the bloodstream), the uric acid crystals will then start to deposit. Uric acid often bonds with other elements to form urate crystals, which the immune system then attacks and produces the typical painful flared joints associated with gout. Urate crystals can also deposit in the skin where they cause gouti tophi, but can also deposit in tendons to produce tendon pain. Treatment of gout involves medicine known as urate lowering therapy as well as a diet low in purine rich food, to allow the levels of uric acid to drop thereby allowing the body to reabsorb the crystals and then allow symptoms to settle.”
One final point, load can still play a large role, even within inflammatory conditions. An increase in tendon symptoms may follow an increase in loading, equally they may also be linked to a flare in the underlying rheumatological condition.
Role of TendonQ – the questionnaire is designed to identify key signs and symptoms of inflammatory joint disease including peripheral or axial spondyloarthropathy. In addition is screens for common extra-articular and peri-articular features detailed above. The aim is not to suggest the form makes any type of diagnosis! It simply helps your reasoning process by identifying (or excluding) specific symptoms.
Diagnosis of inflammatory conditions is complex and requires specialist input and appropriate investigations.
Action points – if you suspect an inflammatory joint disease seek a referral to a rheumatologist, usually this can be arranged via the GP. In addition, requesting a full blood count including inflammatory markers (ESR, CRP etc) HLA B27 and liver function tests can be helpful too. If you can already have the results of these tests prior to seeing a rheumatologist it can save time and help in the diagnostic process.
Medications
Certain medications may play a role in causing or exacerbating tendinopathy;
Fluoroquinolones anti-biotics (including ciprofloxacin and levofloxacin) may cause tendinopathy. Symptoms usually develop acutely after taking the medication (median duration 8 days), patients over 60 are at greater risk and approximately 40% of those affecting the achilles tendon lead to complete rupture (Scott et al. 2015).
Statins – patients commonly report muscle pain in association with statins but around 2% may develop tendinopathy (Scott et al. 2015). However a recent review (Teichtahl et al. 2016) has suggested some statins may be protective against the development of tendinopathy so there is some debate over their exact role.
Steroids – corticosteroids can impair collage synthesis and reduce the sensile strength of a tendon (Scott et al. 2015). Long term use of steroids may increase risk of rupture, especially following tendon injection.
The role of TendonQ – identify key medications that might influence tendon health
Action points – history of taking any of the medications above should make us mindful that an increased rupture risk may be present. A more careful, slower progression of loading should be considered. In addition the psychosocial influence of these medications may be a factor. Some patients may have been told, for example, that fluoroquinolones increase risk of rupture and this may create fear of loading that needs to be addressed with careful reassurance.
The ‘capacity’ changers
This is based, for the most part, on excellent recent work by Scott et al. (2015) referenced above.
A number of factors can influence a tendon’s capacity to manage load and to adapt to it. These include;
- Age – increasing age is associated with reduced tendon strength although this may be counteracted with exercise (Svensson et al. 2016 In Press).
- Peri-menopause – hormonal changes around the menopause, especially loss of oestrogen, are thought to have a negative effect on tendon homeostasis (Hansen et al. 2009).
- Smoking – associated with worse tendon histology
- Thyroid dysfunction – thyroid hormones can influence tendon homeostasis and collagen synthesis but their exact role in tendinopathy is not yet fully understood. Olivia et al. (2013) discuss this complex topic in a little more detail (thanks @AngeloCacchio for recommending this paper!).
- Diabetes – A systematic review by Ranger et al. (2015) reported there was strong evidence that diabetes is associated with a higher risk of tendinopathy.
- Hypertension – has been associated with tendon pain (Abate et al. 2009)
- Obesity and raised cholesterol – Elevated BMI appears to increase risk of both upper and lower limb tendinopathies. Scott et al. (2015 p838) describe this brilliantly and reference their earlier work,
“The biological mechanisms have not yet been established, but excessive dietary intake of cholesterol does result in the accumulation of oxidized low-density lipoprotein in the load-bearing region of tendon, where it impairs type I collagen production and reduces tendon strength and energy-storage capacity. (Scott et al. 2014)”
The role of TendonQ – to identify any relevant factors that may influence the tendon’s ability to manage load or adapt to it.
Action points – If these factors are identified we should consider a more gradual progression of loading. Some factors might be changeable e.g. Smoking and weight. MDT working with the patient’s GP may help ensure peri-menopausal changes, thyroid dysfunction and diabetes are managed optimally. In addition a lipid profile may be useful if indicated.
Psychosocial factors
I think it’s fair to say that current management of tendinopathy is quite ’tissue focussed’. The consensus at present appears to be a structured and progressive loading programme to improve the load capacity of the tendon and kinetic chain. Little research has focussed on psychosocial factors but they can be key in managing tendinopathy.
A growing body of evidence suggests stress may have an impact on healing (Alford 2006) and strength gains and recovery from resistance training (Bartholomew et al. 2008, Stults-Kolehmainen et al. 2007). I’m not aware of any studies specifically on tendons but it certainly seems plausible that stress could be a significant barrier to rehab and may impact tendon adaptation.
Anxiety and depression have also been found to influence pain and coping strategies (Gerrits et al. 2015) and could also be an important factor in tendon pain. Lack of sleep may influence pain (Finan et al. 2013) and has been linked with increased injury risk (in adolescent athletes – Milewski et al. 2014) and impaired performance in athletes (Marshall and Turner 2016).
Slide courtesy of @DerekGriffin86
Recent research (Forsdyke et al. 2016) has highlighted that how we think, feel and behave will influence the outcome of rehab following sports injury. A positive perception of return to sport has also been associated with a greater likelihood or returning to a pre-injury level of sport (Ardern et al. 2013). While work specific to tendons is sparse in this area emerging evidence suggests it could play an important role. Green et al. (abstract only) examined adherence to the Alfredson eccentric exercise programme. They identified that negative beliefs about the condition and fear of tendon rupture could reduce exercise adherence. It’s important to note that this is a small and, to date, unpublished study of just 5 patients but it may provide some indication of the impact of beliefs on rehab.
Role of TendonQ – to identify any previous history of mental health and provide a picture of current mental wellbeing and psychosocial factors that could influence rehab.
Action points – the questionnaire may provide clues to psychosocial factors but a more in-depth discussion of identified areas is warranted for each patient. This allows us to guide the patient on making lifestyle changes, educate and reassure where needed and involve other members of the MDT as required.
For more information about the treatment of tendinopathy and other common running injuries book on the Running Repairs Course. TendonQ is the first of a number of projects designed to help therapists and health professionals in clinic.













Thanks ever so much for compiling such excellent piece of work.
May I ask whether there is ref as to the relationship between gout and tendons? and how it might affect prognosis?
Comments are closed.