Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
The Glutes have enjoyed much of the limelight in running articles in recent years. Indeed our most popular post remains our discussion of glutes exercises. While the glutes certainly have a role in injury treatment and prevention they can also be a source of symptoms in their own right. This article examines one such problem – Gluteal Tendinopathy (GT).
This piece is based on excellent work by Dr Alison Grimaldi who has a free PhysioEdge Podcast on the topic as well as great published work she has kindly made available on her website. Alison was also very helpful on Twitter and discussed some of the issues surrounding this condition – some of her comments from this discussion have been used to inform this article. The full discussion can be found here and you can follow Alison via @AlisonGrimaldi. Her work has been combined with studies from Angie Fearon and seminal tendinopathy research from Jill Cook and Craig Purdam.
If you’re a Physio and you’d like to find out more I recommend Alison’s new online course and 1 day practical – Tendinopathies of the Hip and Pelvis (online component can be done as a stand-alone course for those unable to attend the practical)
Signs, symptoms and pathology
GT typically presents as pain over the greater trochanter (the bony lump felt at the side of your hip). symptoms may spread into the outside of the thigh and knee. It is commonly misdiagnosed as hip joint pathology, ITBS, sciatica or as being referred from the lumbar spine. GT is a good example of how clinical knowledge has progressed in recent years. Initially, it was thought of as inflammation of the trochanteric bursa – a fluid-filled sac that sits over the trochanter. However, as research developed we realised 2 rather important things. The bursa may not be the issue and there isn’t really any inflammation. Later the condition was termed Greater Trochanteric Pain Syndrome (GTPS) but further research has enabled us to be more specific with the diagnosis. Bird et al. (2001) examined MRI findings of patients with GTPS, they found that nearly all patients had evidence of Gluteus Medius Tendinopathy. Swelling of the bursa was present in just 8% of cases and did not occur in the absence of gluteal tendinopathy.
The primary pathology of Gluteal Tendinopathy is most likely insertional tendinopathy of the Gluteus Medius and/ or Gluteus Minimus tendons and enlargement of the associated bursa.
Picture from Williams and Cohen (2009) freely available online here.
Most recent theory suggests that this tendon is compressed by the Iliotibial Band (ITB) when the hip is adducted (which happens when the leg moves in towards the other leg). This compression can be increased if combined with flexion or external rotation of the hip. Recent work by Cook and Purdam (2012) has highlighted the role compression has in tendinopathy.
Tendon structure is well suited to manage tension – it has ‘viscoelastic’ properties which allow it to work like a complex spring to deal with load. It can manage some compression too – areas of the tendon that are prone to compression develop a slightly different structure that is similar to cartilage found in joints – however, it’s fair to say it that generally tolerates tension better than compression. Perhaps the biggest issue for tendons is when both types of load are combined and the tendon is under both compressive and tensile load simultaneously. If this excessive load continues the tendon reacts by swelling to ‘stress shield’ the tendon. However, this increase in tendon size can lead to more compression and usually results in pain. If this overload continues in the long term the tendon structure starts to suffer leading to tendon disrepair and eventually degeneration. In the case of some tendons, including the gluteal tendons, this can lead to tendon rupture.
Gluteus Medius and Minimus anatomy reproduced from Gottschalk et al. (1989) freely available online here.
How does this relate to GT?
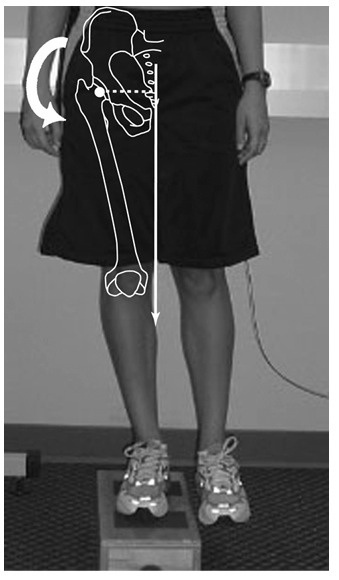
The key variable appears to be hip adduction. The hip can be adducted by moving the leg across the midline and if the pelvis on the opposite side drops during weight-bearing activity. This means the hip is adducted relative to the pelvis (see pic below reproduced from Bolga 2005). If this hip is flexed as well as adducted this can add to the aggravation. So If you have GT it’s likely that your symptoms will include pain with crossing your legs and with climbing stairs or hills, even just with single leg balance if your pelvic control is poor. Each case is different though and in milder cases, these may be fairly pain-free. For runners, it’s likely to be painful during the impact phase of running when your foot strikes the floor and your bodyweight moves over the foot. If movement control is poor you may find your hip adducts slightly during this phase. This combines both tensile and compressive load and is likely to cause pain in GT. Running on a camber (such as on the side of the road) can exaggerate this hip adduction and aggravate symptoms further, in some cases even walking on a camber will also be painful. Gluteal Tendinopathy is more common in women than men and is common in postmenopausal women. Fearon et al. (2012a) found an association between ‘adiposity’ and GT in women and found ‘lower neck-shaft angle’ was a risk factor. Leg length discrepancy and spinal scoliosis have also been associated with GT.
One other key characteristic with GMT is pain in side-lying. Unfortunately, it can be painful on either side making sleep very difficult. The issue is if you lie on your painful side there is likely to be some direct compression of the gluteal tendons. If you lie on your good side the bad leg is uppermost and often falls into adduction and flexion. Considering we spend some hours sleeping this can be a significant source of aggravation for the tendon.
While hip adduction is a key factor but I don’t want to demonise it too much! Hip adduction is a normal movement, sleeping on your side is fine in a normal situation. The issue is when the tendon has reacted to load and swollen it can be sensitive to even relatively small amounts of compression leading to pain. If we keep aggravating this tendon in compressive positions it’s unlikely to settle.
Is it Gluteal Tendinopathy?
Diagnosing GT is not straightforward – the hip is a complex area and there are a host of other potential diagnoses. In addition, GT is often seen alongside other hip pathologies and can present with low back pain. Tortaloni et al. (2002) found that 20% of those referred to a spine specialist had GT.
If you have persistent pain in the hip region see a medical professional for assessment, diagnosis and treatment.
It is possible for several conditions to present at once but generally GT wouldn’t present with pain down the entire leg as far as the ankle or pins and needles/ numbness. It may present with back pain but the main core of the pain will usually be over the greater trochanter in GT. This is a key part of the diagnosis. Aggravating movements are more likely to be related to hip movements, especially ones involving adduction as detailed above. If your pain is more centred around the lower back or is aggravated more by back movements it is less likely to be GT.
Osteoarthritis of the hip and GT can easily be confused, and may present with pain in similar areas. Typically OA of the hip may be more likely to include groin pain and restricted movement of the hip joint but if diagnosis is unclear an X-ray may be indicated to help rule out OA. It is also possible for these 2 conditions to co-exist. Fearon et al. (2012b) compared Greater Trochanteric Pain Syndrome (GTPS – another term for GT – to avoid confusion we’ll stick with the abbreviation of GT) and hip OA, they found a trend for GT patients to be younger (on average 53.8 years old for GT and 62 for OA). That said they found just 2 key factors that were significant in differentiating between OA and GT; the ability to manage socks and shoes and the FABER test (detailed below).
So if you have pain over the greater trochanter but have no difficulty managing socks and shoes with a positive FABER test it’s significantly more likely that you have Gluteal Tendinopathy than OA of the hip.
Your Physio or GP will assess the area and do a number of tests. Within these are a few key tests to assist diagnosis. Alison Grimaldi describes 2 tests for GT – 1) combining hip adduction, 90° flexion and external rotation and 2) a modified ‘Ober’s test’ which involves adducting the hip in side-lying. Both are likely to cause compression of the gluteal tendons. These tests can be modified by palpating the tendon in this position or resisting internal rotation of the hip to work glute med. These additions can be used to further confirm diagnosis of GT if the initial test is only mildly painful. The work of Angie Fearon (detailed above) would also suggest adding the FABER test to differentiate between OA and GT;
Staging the tendinopathy
Excellent work by Cook and Purdam (2009) has helped us understand different stages on tendinopathy and how to treat them. Broadly speaking we consider there to be 2 stages seen clinically – reactive (and early disrepair) and degenerative (and late disrepair). More here on staging of tendinopathy. I discussed staging of gluteal tendinopathy with Alison Grimaldi and she said it’s easier to stage patellar and achilles tendinopathy as they have an inherently more simple structure and that load management is crucial at any stage in GT.
The reactive stage is usually an acute response to excessive load. If you’ve increased or changed your training and you have pain as a result this is more likely to be reactive, especially if you’ve had no issues before. Change in training might be longer distance, adding in hills or doing step aerobics all of which can lead to a combination of compressive and tensile load on the tendon causes a reactive response.
If you’ve had grumbly lateral hip pain for a while which has progressively worsened and you’re an older athlete then it’s more likely in a degenerate stage. However, given the complexity of gluteal tendinopathy it’s hard to make this diagnosis without examination and appropriate imaging.
Management
Reactive/ early disrepair
Arguably the key treatment strategy in reactive tendinopathy is reducing load on the tendon to a level that stimulates recovery rather than symptom aggravation. Compression of the tendon or activities that require the tendon to behave like a spring (known as the stretch-shortening-cycle) are likely to aggravate a reactive tendon. Activities that combine both these loads are likely to be especially provocative…

Picture source
…so what should you be careful with – the key factor is adduction of the hip (the movement where the leg moves in towards the midline, such as crossing your legs). If this is combined with flexion of the hip or a lateral tilt of the pelvis it can add to the compressive element. Any movements that increase tension on the ITB or structures that attach to it (such as TFL) are likely to increase the compressive load.
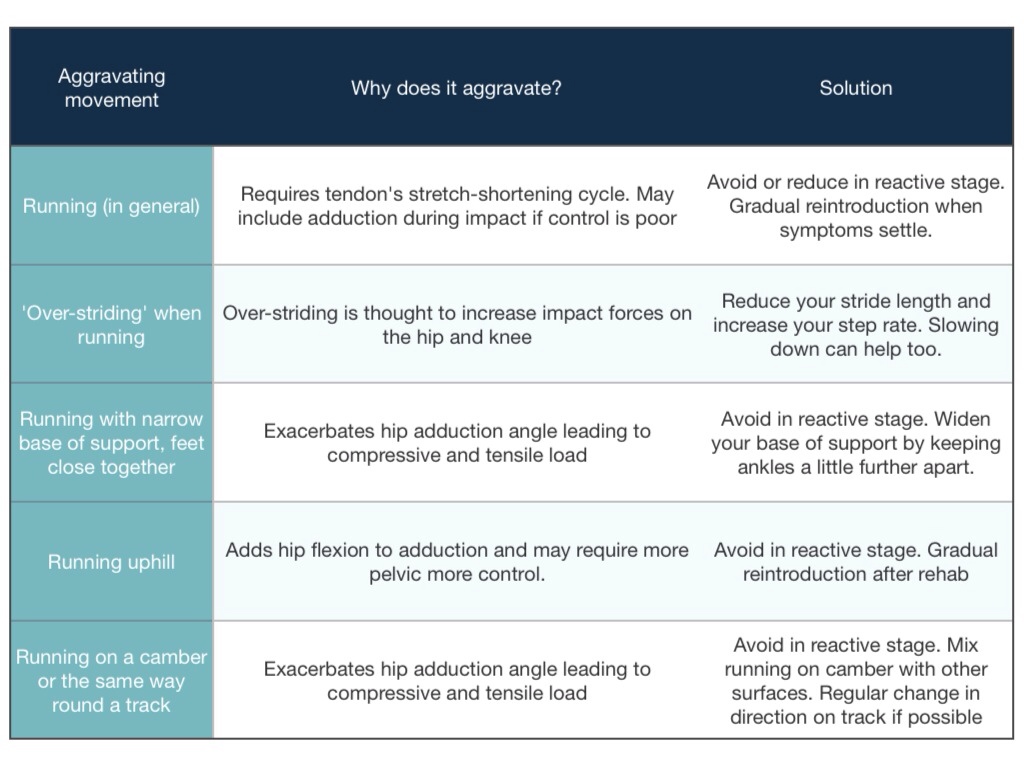
The tables below show activities that can be modified to reduce load on the gluteal tendons. We rarely recommend avoiding activities altogether but rather ‘pacing them’ – this means modifying them or reducing them to a level the tendon can manage. If some movements are especially provocative you may choose to avoid them initially but this should only be a short term measure. Generally, your guide is to see how activity affects your symptoms a) in bed at night and b) the following morning. Aim to find a level of activity that doesn’t provoke symptoms at these times.
During the reactive stage of tendinopathy the tendon swells, this can make it more vulnerable to compression and exacerbate the problem. By ‘pacing’ these activities the tendon is able to recover and gradually the swelling and pain will reduce. How quickly this happens depends on the severity of the tendinopathy, it’s causes and how much you are able to reduce aggravation. In mild cases, pain may reduce within the first 5-10 days but these problems can linger and tendon healing is generally slower than other tissues. In some cases, it may take 3-4 months to settle.
Another consideration in the reactive stage is non-steroidal anti-inflammatory drugs (NSAIDs). Although tendinopathy is not an inflammatory pathology NSAIDs are thought to help by reducing tendon swelling. Cook and Purdam (2009) recommend ibuprofen as an option as it’s thought to help without having a negative impact on tendon healing.
Always discuss taking new medication with your GP or pharmacist, NSAIDs have a range of side effects and are contraindicated in a number of conditions.
Isometric exercises are thought to be helpful in the reactive stage, however, these need to be done correctly to avoid increasing tension on the ITB. An issue here is the TFL muscle, it can be overactive in abduction activities. If when doing these exercises you work TFL rather than Gluteus Medius and Minimus you may well exacerbate the problem. It’s also very important not to do these exercises with the hip adducted. There are a host of glutes exercises but some I would avoid for this condition – these include ‘the clam’ and ‘pelvic drop’ (detailed here in glute med exercises). It’s important to progress to weight bearing but single-leg activities (such as single leg balance and single knee dip) should not be started until you have adequate pelvic control. Alison Grimaldi discusses exercises in her PhysioEdge podcast – a good starting point is isometric hip abduction in side-lying (pictured below). This be achieved by lying on your good side with your painful hip supported on pillows so it rests in a neutral or slightly abducted position. Start by trying to lift some of the weight of your leg off the pillow and hold for 10. Progress to lifting the leg 1-2 cm off the pillow and holding. You should feel the muscle working just above and behind the greater trochanter rather than down the side of the leg. This isn’t an easy exercise to get right, in fact many of the glutes exercises are easy to get wrong!…
The best advice is to see a Physio who can assess you and provide appropriate exercises and help you perfect the technique. They can then help progress your exercise into functional weight-bearing positions and help identify other potential causes of GT.
Assessment and rehab of single leg balance – focus should be on maintaining a level pelvis without adducting the hip. Use support initially if needed. Aim for 10-15 seconds, repeat 5-10 times (stop if painful).
Running may need to be avoided or at least reduced during reactive tendinopathy. This is the last thing you want as a runner but maybe a necessity in early management of GT. The issue with tendinopathy is that if you continue to overload the tendon it can progress from a reactive tendon, to dysrepair and degeneration during which stages the tendon structure starts to change. Reactive changes are reversible but degeneration of the tendon generally isn’t. That doesn’t mean it can’t be managed it’s just better to prevent it happening in the first place!
In mild cases, you may continue to run but try to ensure running remains pain-free and there is no reaction for at least 24 hours after. Your Physio should guide you on continuing to run and/ or returning to running after rehab. In achilles tendinopathy Silbernagel (2007) demonstrated that continuing to run didn’t have a negative impact on recovery as long as runners didn’t allow pain to increase above 5 out of 10 (where 0 is no pain and 10 is the worst possible pain) and symptoms had settled by the next morning. The study included only achilles tendinopathy, and only people who had symptoms for at least 2 months so I would urge caution in applying it to GT. Any return to running should be gradual and avoid hill work and speed work initially.

Late dysrepair/ Degeneration
Many of the principles of treatment remain the same during the dysrepair/ degeneration phase – load still needs to be modified by reducing hip adduction and ITB tension and pacing of aggravating activities remains useful. However, NSAIDs are no longer likely to be effective and exercises can be progressed and may include heavy loading or eccentric work (but only if adequate control is achieved). These exercises should be provided and demonstrated by a Physio to ensure the deep gluteal muscles are working rather than superficial muscles such as TFL.
The mainstay of managing gluteal tendinopathy regardless of stage is reducing load on the tendon and improving control of hip and pelvic movement. Other treatments may be added to this as long as they assist this process.
Other treatment options
Stretching
Don’t stretch your glutes or ITB. This is vital as it will increase tendon compression. There is some debate on the benefit of stretching and whether is can achieve tissue length changes. The safest choice for GT is not to stretch. If your ITB or TFL feel tight or have ‘trigger points’ gentle self massage may be helpful. You can try using the foam roller but only if you do so without adducting your hip and it doesn’t aggravate your symptoms. There is no direct evidence I’m aware of showing that using a foam roller will help GT but it does have the potential to aggravate it. Direct tendon compression from the roller will aggravate and the action of the roller can cause a ‘bowstring effect’ increasing muscle tension. It might be best avoided or used very sparingly.
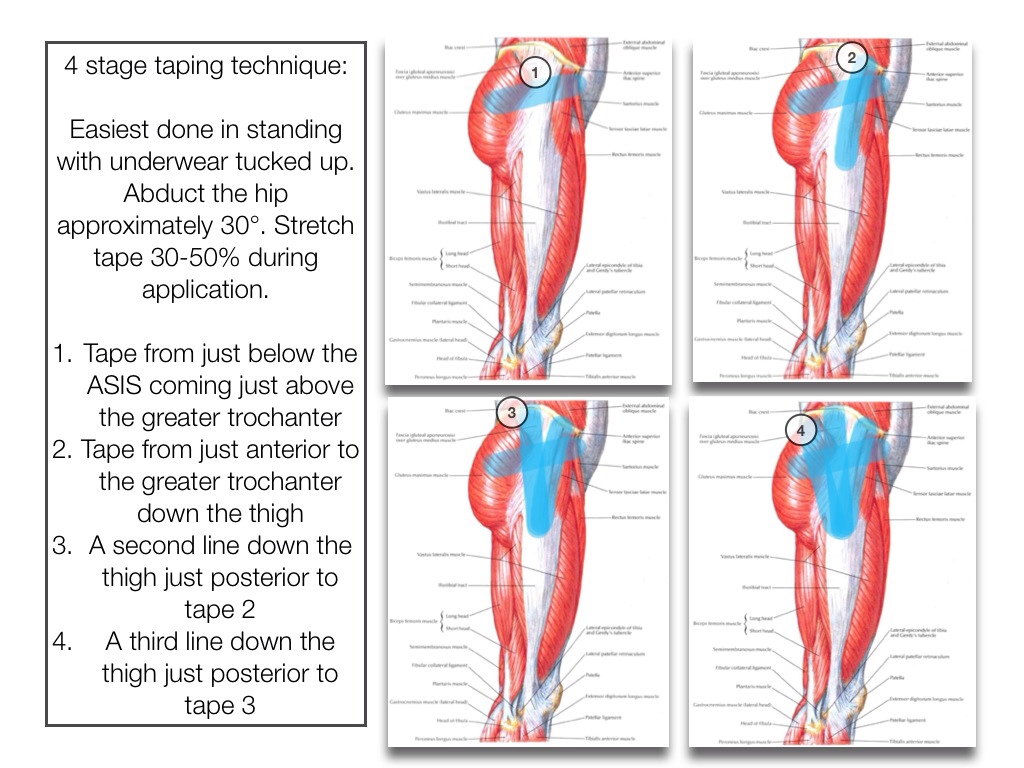
Taping
I have used a Kinesio taping technique for this condition that seems to help in the clinical setting however I’m not aware of a single piece of research that’s examined the use of taping in GT so recommending it is in no way evidence-based! The technique is described below. The aim is to provide some extra lateral pelvic stability, whether a tape can really achieve this is certainly debatable but it does seem to achieve one thing very well…it stops people crossing their legs! The tightness of the tape on the outside of the the thigh makes adduction difficult and if nothing else works as a little reminder to stop people spending prolonged periods in an adducted position. It’s not research-based and I would opt for activity modification first and foremost but taping is something I’d file under might be worth a try. If it’s uncomfortable or aggravates your symptoms then remove it.
Closing thoughts: Gluteal Tendinopathy is a complex condition but one that can be treated with management of tendon loading and rehab of movement control. Alison Grimaldi’s research has raised important questions about how we work the gluteal muscles. While EMG studies have been helpful in this area they may only identify how to work superficial muscles and not how to normalise muscle function in a condition like GT.
If you have Gluteal Tendinopathy I recommend seeing a Physio or health care professional for detailed assessment and advice, especially on exercise selection. As ever on RunningPhysio, if in doubt get checked out!
Further reading:
Grimaldi (2011) – a detailed discussion of lateral stability of the hip and pelvis
Reiman et al. (2012) – systematic review of EMG studies of Gluteus Medius and Maximus – discussed on RunningPhysio here. It should be noted that many of these exercises would not be appropriate for Gluteal Tendinopathy either due to excess hip adduction or tendency to recruit more superficial muscles.















Hey Tom
Another cracking piece, love the new image layouts, the content ain’t to bad either… Lol
One little thing, you know me always have to say something,
I think that although our understanding of lateral hip/leg pain is improving it seems that certain structures go in and out of favour as often as the seasons, and depending on who ever is the darling of the research world this month!
The role of the bursa as a pain generator has gone right out of fashion in recent years in favour of the glute tendon and yes I agree the glute tendon is regularly a problem here, but so are the bursa! Controversial I know its almost seen a crime now to dare say bursitis in physio for fear of being flogged and told to stand in the thick corner… I’m usually found there!
The lack of seen bursal effects eg, free fluid seen on MRI USS doesn’t mean the bursa isn’t causing pain, we know from histological studies on the sub acromial bursa that bursa are very, very, very, very richly innervated and generate heaps of pain, even without observable signs, this recent paper on sub acromial bursa backs me up on this http://www.ncbi.nlm.nih.gov/pubmed/?term=Why+does+my+shoulder+hurt
Speaking from experience I have seen these lateral hip pains help greatly with USS guided bursal CS injections and then the physio rehab you so excellently describe above, but it seems that injections here are rarely recommended anymore due to it going out of favour with injections being seen as aggressive and invasive and bad blah blah, this I think is a mistake, yes we shouldn’t be pumping everyone immediately with corticosteroids but they help immensely when given at the right time, in the right way and most importantly in the right place
Anyway to wrap it up before I go on and on, I think the bursa are important and yes the biomechanics and tendons are also too but we should rule out injection therapy to help in this condition just as we do in sub acromial shoulder issues to reduce pain which then helps improve movement and ultimately helps physio
Sorry for going on and on, great piece again, top draw stuff
Cheers
Your No1 fan
Adam
Thanks Adam, you always bring an informed perspective to these discussions! I agree perhaps we tend to throw the baby out with the bath water and too rapidly abandon treatments. That said I’m not well versed in the literature on injection of the various bursa around the hip, perhaps the results have been especially poor?
I think load management and improving pelvis and hip control remain first choice treatments. Perhaps injections should remain an option if these approaches fail?
Cheers
Tom
Hey guys,
Thanks for bringing sense to these collection of articles and publicising Alison Grimaldi’s work. I think she makes a great contribution to our understanding of this particular tendon disorder.
I am an ESP physio who injects and I think that there is an arguement for its ‘judicious’ use. I see plenty of patients, usually women, 50’s plus who don’t run but who are in incredible pain and are suffering with this pathology. My colleagues try to off load, decompress with positioning etc but if the tendon is swollen, torn, disrupted, thickened, calcified or other…injections do have a place to provide a window of opportunity for rest, and reloading. I have seen it work, but cases should be considered individually. I know that steroids have a bad rep but they do have their place for very painful conditions when there are no other modalities helping the patient.
Also, I think it is interesting to note that Alfredsons eccentric loading programme is designed to treat mid tendon achilles tendon problems and not insertional ones, therefore if glute tendinopathy is a degenerative tendon pathology aggraved by intrinsic problems of angiogensis and compression, perhaps re-loading needs to looked at more carefully.
It is a really exciting area this ‘rotator cuff’ of the hip… I am sure we will struggle on with managing tendon problems..
Finally note, I think anyone with a tendon problem needs to think of time frames of 6 months to recovery and that is if they follow the programme but also to note that even then some people will continue to struggle with symptoms.
Final, final note, any thoughts on autologous blood injections for this region. They are used in sports medicine but I have heard much of their use for this particular pathology
Hi Matt, I have been diagnosed with GT and I am wondering if you would have some for my questions on injections for this particular condition?
[email protected]
Regards, Reece
Hi Tom
You referred a runner to me in Preston
I have seen him and he does in fact have a greater trochantor pain syndrome
My assessment tips
Testing: External de-rotation test, positive jump sign, single leg stance test
Muscle length – thomas, ITB, Gastroc/soleus, hamstrings
Muscle testing: Clam and hip abduction static – can they maintain full inner range
Clam and hip abduction dynamic – non loaded with control if they hit 30 with ease (they won’t) add weight either theraband or ankle weight around knee.
Single leg bridge – static timed and dynamic fatigue
Side plank 1/2 lever, full lever timed
3 way assisted sit up control using theraband
Squat – biomechanical faults – Trunk deviations and lumbar flexion give, hip IR and add, knee valgus collapse, knee too far over toes, ankle equines, rear foot valgus – if they pass this then:
Lunge with same biomechanics – if they pass then
assisted single leg squat – then
single leg squat – with same biomech control
then we start to go on to load acceptance work like squat jumps and single leg squat jump control with correct biomechanics – then onto plyometrics and sports specific
obviously don’t go through all this with your weekend warriors if theyre in agonising pain
cheers
Matt (unfortunately I know Richard Norris)
Hi Tom
I have this problem with laterel hip pain around the greater trocanter, but I also have a very tight itb. If I put my hip a littel bit out to the side, it snaps around the greater trocanter. I try to avoid compression, and gentle try to improve my muchel strengh around my hip. I dont strech my itb, but my worry is, have I can get the itb longer, when I don´t strech? Do yoy have some advice about that?.
Best Wishes
Kristine
I have had bilateral gluteus medius tendonopathy for about two years now. It was diagnosed through MRI. I was an avid cyclist, hiker, and I also did regular weight training. The orthopedic doctor gave me no advise on treatment, so I began physical therapy, but that made it worse. I have had to give up all activities because of the severe night pain.
I recently bought the Q1000 cold laser with a probe attachment and it has been remarkable. It completely takes the pain away within about five minutes. I am not yet back to activities because I’m afraid of re-aggravating the condition. I would love to see if this laser just takes away inflammation or there has been some actual cellular healing.
Has anyone else had experience with a cold laser?
Hi Susan. Where can you buy the Q1000 cold laser, and what is the price? Are you still pain free? I also have this problem, and had for a long period, so I am very interested in hearing more about it. Best wishes Kristine from Denmark.
Sorry for the delay in response. I bought the Q1000 laser on line. I also bought the 808 probe because it was recommended for joints. It does work well for pain relief and reduction of inflammation, however I am still dealing with this issue after 3 years. The probe and laser were about $5,000.
Hello – thanks so much for the info regarding the gluteus tendinopathy. It was really good information and I really appreciate it. Do you have any thoughts on doctors or physical therapists that are specialist in this area in the Washington DC area or down In Charlottsville VA? As I have seem to have met a bunch of incompetent people. I had a laberal tear which was repaired and they thought my hip pain was caused by that. The doctor cut right into the area where it was aggravated as well. I have had this for five years now. I went to physio, chiropractor and pain doctor who recommended using the roller to loosen IT band. Although that is tight the MRI says mild trochanter bursitis and gluteus tendinopathy at insertion point. I’m afraid they may have done more damage as the pain doctor recommended using the Graston Technique on me so I went to the chiropractor. He would rub that metal instrument along my hip and IT band causing a lot of bruising. Also, when I first had the problem the physical therapist would take this stick and rub my hip bone and stuff it was very painful and I wasn’t sure if she should be doing that. Then I went to another physical therapist who put my leg across my body when I told them I was unable to adduct or abduct for three years without pain. Then another pain doctor told me I just needed to work through the pain. I’m wondering if these people did more damage then good. I also had three PRP injections at $500.00 a pop which did little. I’m in constant pain – especially sitting. I’m willing to travel but nobody seems to know what they are doing until I read your article above. I can no longer walk long distances, running – not at all, no weight lifting with the lower body, ballroom dancing. And sitting is the worst – work is very difficult. Mainly just lay on the couch. Very discouraging as I used to be such an active person.
I have had a similar experience. MRI showed gluteus mediums tendonosis. I have struggled for 18 months with pain and the doctors and pt’s ignore the pain side lying and crossing my legs. They continually treat my back including doing epidural injections. Nothing has helped because they are not treating the problem. I only hope I haven’t done more damage with the physical therapy. Does anyone know any good doctors or pt’ s in the detroit area.
Hi Jennifer Smith,
Were you able to locate good doctors to help you with your condition? Looks like I’m experiencing the same exact thing — lots of incompetent people, I’d love to hear if you are feeling better and who/what helped.
Hi Paul,
No I never found anyone that could help me. Dr. Grinaldi didn’t know of anyone in this area. Basically still feeling bad. Ibuprofen helps. Yesterday it felt okay so I tried slow jogging which I hadn’t done in a long time. It gets aggravated especially the next day. That was the trouble with me – I’d try and do what they’d say and sometimes it wasn’t while I was doing it but the next day would be all aggravated.
So sorry, and I totally understand. I have had this problem for 3 years now. My first MRI revealed tendonopathy of glute medius and minimus on both sides and greater trochantic bursitis. I did rehab which helped somewhat. I bought a Q1000 laser with probe, this also helped somewhat. It did at least stop the pain at night. I have not been able to get back to walking or cycling.
I just had a second MRI and saw a different doctor. This MRI revealed psoas bursitis and rectus femoris bursitis. There was no mention of the tendonopathy. Neither of these doctors seemed interested in giving me a consultation, so I am on my own trying to set this right.
The biggest help so far has been releasing trigger points by laying on a tennis ball. The second doctor wants to inject the bursas with cortisone. I am not ready to do that based on my research. I have just read about using DMSO. that looks very promising and I have ordered some. I have used it extensively with horses. I think continuing with stretching and strengthening is key. I will let you know about the DMSO. I have also bought a home ultrasound unit. That has also helped with pain.
Jennifer Smith — If you’re still looking for a good physical therapist for this condition in the Washington, D. C., area, I’ve been impressed with Michael Uttecht at Medstar Georgetown University Hospital.
Great site Tom! What a nice patient friendly description in addition to provision of differential diagnosis for this hip pathology. Thank you for helping folks decipher the difference between OA and Glute tendonosis.
Regards,
Amanda Olson, DPT
Hi Tom,
Interesting stuff.
I have recently got MRI results which confirm glute medius tendonosis, Would you advise that I hit it with eccentric work or eccentric/concentric? I was thinking of monster walks, with a band, using the good leg to load, or side lying slow adduction, with a pulley to load?
My physio suggested eccentric and concentric, but based on my experience with tennis elbow, it should be eccentric only?
Thanks Mick
[…] I have now scrapped this exercise, It is compressing the gluteal medius and should be avoided: Running Physio […]
[…] He basically reiterated this: http://www.running-physio.com/gluteal-tendinopathy […]
Finally some confirmation of what I have been saying about myself. Walking makes it hurt, biking does not. It hurts more at night and in the morning. Meloxicam is not helping. The exercises make it worse. The stretching hurts. I have not seen my PT in 3 weeks, because the exercises were not helping, nor has the cortizone shot done anything. I see the psy med doc Monday and I will be bringing this info with me. I am not crazy. These are exactly my symptoms and exactly the things that make it hurt worse…crossing my legs, standing too long, sleeping on my side–even with the pillows, but less with the pillows. Thank you for this information, I was beginning to feel like a Hypochondriac. This has been going on for 10 years. TEN years.
My story exactly. This week I finally figured it out for myself and I am 80% better.
I Found articles on trigger point referral patterns. My problem is trigger points in the psoas muscle and trigger points in the glutes. I manually released the trigger points in the psoas( the major muscle for walking) and used a tennis ball on the 3 glute muscles. Unbelievable.
Very interesting reading for me too and I am freaking out that after almost 6 years of unsuccessful treatment approaches, is my tendon going to have entered the degenerative phase? How can I find out about this? I am planning a Skype consult with Alison Grimaldi in the next few weeks but keen for other opinions too!!
Hi Amanda,
Also had this problem for years, let us know how you get on with Alison. I currently feel like I am improving but progress is slow.
https://glutealtendinosis.wordpress.com/
Mick
Hi Mick, sorry for slow reply, I have had 3 Skype consults with Alison now and focus is totally on recruiting deep stabilising muscles and avoiding any irritating activities. So she retired me from running and biking and it’s been mentally very tough. Unfortunately nobody can tell me how long I have to keep ‘rehabilitating’ when I have had 6 years of issues
I’m getting steroid injections in a couple of weeks. Seen lots of different physios and nothing is working, so need to do something different.
Hi Amanda,
I have a very similar situation as you but mine has only been going on for two years, its slowly been getting worse and i can no longer walk or do any exercise.
Would you be able to share what exercises Alison has given you?
Also how is your pain now??
Thanks,
Daniel
Thank You very much for making me aware of this diagnosis. I finally have something to hope for. My doctor said I am just depressed and imagining the symptoms and that there is nothing wrong with my hip (since it was not bursitis). I live in Finland and it is sad to see how ignorant our doctors are. “Jortse”
Please can anyone reccommend a physio in UK preferably south west who knows how to deal with this ?
I have seen 3 osteopaths and a physio so far none of whom seem to have the Grimaldi knowledge and I desperately need some proper help to see whats going on and how to get back to normal.
I sit and cry some nights from the pain and hopelessness.
Please help ? Thanks
[…] http://www.running-physio.com/gluteal-tendinopathy/ […]
Oh, wow, I am bummed to see my thoughts reflected in these posts. I have feared that this was going to be something very difficult to manage–I have been doing nothing but lying around for two months and seeing my chiro for trigger points–deep in the priformis and other muscles– but have had zero relief. I am hoping I have a tear, because that can be repaired, but I have had gnawing dread that it is degenerative. It is so painful! I have to fight every day to stay upbeat. I used running–just 2 or 3 quick miles every other day–to manage lifelong depression and anxiety. plus I walked fast everywhere, and was on my feet most days. With this inactivity I feel like I am suffocating..ugh.
Thanks and best to you all. Hope to hear more of your ideas and experiences. It is very helpful.
Marcy
Oh, yes and I found a helpful way to rise from a seated position–in fact it is the only way I can! Without adducting my legs, I manage to get to the edge of the seat. Then I grip the very top of my thighs and push downward an inch or two toward the knee, as if I were going to do a deep massage. Still pushing in and downward, I lean forward and down, raise my rear off the seat and slowly straighten my legs while still facing downward. Then I straighten up to standing. Pretty pitiful for a runner, eh. But I can do it pretty quickly now. (what a relative term “quickly” has come to be!)
Marcy
I have been suffering from glut. med. pain for over 30 years and one time I was diagnosed by ultrasound imaging of having glut. med. tendinopathy. Running has been difficult. I read this article in 2013 with interest, and it was of great help. Including massage by a professional therapist twice monthly with emphasis on the hips and exercises as described in this link http://www.cyclingphysio.com/gluteus-medius.html I now do 100 km per month without much hip problems. In fact, nowadays I experience other issues, such as beginning compartment syndrome etc. The amount of suffering seems constant! :=)
Keep Running The Distance
Ing
Can you direct me to any site which has good descriptions, preferably with diagrams, of the types of exercise you recommend for gluteal tendinopathy?
I have been suffering with this for nearly 2 years and have just been diagnosed with gluteus medius and minimus tendonitis and associated trochanteric bursitis following an MRI. I am due to have ultrasound guided steroid injection today. I want to do the right exercises after this, assuming a few days rest first. I have been to a physio, but she is not specialised enough in this condition and indeed doubts the diagnosis despite the evidence. My symptoms match EXACTLY the description in this article. I have a good Pilates teacher, who seems to understand this condition quite well.
I am concerned that due to the time elapsed before diagnosis the condition may have moved on from the reactive to the degenerative phase. I need to look up prognosis for this.
I took up running about 10 years ago when I was 44, but have been unable to run without pain for 2 years now and have had to stop. I try to get out for a flattish, rather slow walk for an hour or so every day to maintain some degree of fitness, but I am frustrated by being in pain doing even this and not being able to do more intensive exercise, especially as I am trying to shed the weight gained when I stopped running. It’s very difficult; sleeping disturbed, unable to carry anything upstairs because I have to hold the handrail, unable to walk up hills, unable to dress standing because I can’t weight bear on the affected side, discomfort sitting.
Thank you for the detailed information in this article and the helpful advice about what to avoid. I need rather more than this though, if I am to overcome this problem.
Does anyone know of a physiotherapist in Kent, UK, who specialises in this condition please?
Comments are closed.