Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
Thanks to the hard work of some excellent research teams we’ve seen several key gluteal tendinopathy (GT) studies arrive almost at the same time! In this series we’ve already discussed the LEAP Trial and interesting research suggesting psychological factors may be important in GT. Today’s blog examines a new randomised controlled trial (RCT) just published in the Journal of Women’s Health comparing gluteal loading and sham exercises for GT. We know from studies in achilles and patellar tendinopathy that loading appears important in rehab so surely the targeted exercises will out-perform the sham ones, won’t they?!…
Ganderton et al. (2018) recruited 94 post-menopausal women with Greater Trochanteric Pain Syndrome (GTPS is also known as gluteal tendinopathy). They were divided into 2 groups with both groups receiving education on activity modification and reduction of activities thought to lead to tendon compression. One group also performed the Gluteal La Trobe exercise programme (GLoBE) while the other had a sham exercise intervention.
The GLoBE programme is clever in its design. In their earlier research Ganderton et al. (2017) examined Gluteus Medius and Minimus muscle activity during rehab exercises in post-menopausal women. This suggested the hip hitch exercise and its variations activate these muscles and may be useful in rehab in this population. It was used within a 4 stage programme beginning with isometric exercise that aimed to load the glutes alongside other important muscles in the kinetic chain (quads and calf);
Stage 1
- Hip hitch (isometric hold, up to 40 seconds)
- Double leg wall squat
- Double leg calf raises
Stage 2
- Hip hitch with toe tap
- Sit to stand
- Calf raises with toe taps
Stage 3
- Hip hitch with hip swing
- Sit to stand with split stance
- Single leg calf raises
Stage 4
- Single leg squat
- Step up
- Single leg calf raises
Dynamic exercises were 2 to 4 sets of 5 to 15 reps (depending on the individual). Further details of the exercise prescription and progression can be found HERE on the Australian New Zealand Clinical Trials Registry.
The sham exercise intervention used a similar dosage and a 4 stage approach but the exercises were not aimed at therapeutic loading of the gluteal tendon or the kinetic chain;
Stage 1:
- Seated gluteal squeeze
- Quads over fulcrum
- Seated calf raises
Stage 2:
- Seated hip abduction
- Seated knee extension (no resistance)
- Seated double leg calf raise
Stage 3:
- Standing lateral flexion
- Seated knee extension against red resistance band
- Seated calf raise with toe taps
Stage 4:
- Standing lateral flexion
- Seated knee extension against green resistance band
- Double leg seated calf raises with pulses up and down
Outcome measures included the VISA-G (gluteal tendon questionnaire) and questionnaires on hip pain and function, global rating of change and quality of life. Data was collected at baseline and at 12 and 52 weeks.
The results
Both groups improved significantly in all measures (except the sports subsection of one questionnaire) from baseline to the 12 and 52 week time points. There were no differences between the groups receiving either the sham exercises or the GLoBE programme designed to load the glutes and kinetic chain.
A responder analysis was performed on those that had a global rating of change of plus 5 or more. In this subgroup (corresponding to roughly half of each group) there were differences between the groups with the GLoBE intervention performing better in most outcome measures at both 12 and 52 week time points.
In addition, it’s important to note the almost half of the participants of the trial were no better, in terms of pain, at the 52-week stage.
Discussion
The study concluded that education (and other factors) may be responsible for the improvements seen in both groups and that type of exercise intervention did not appear to affect results. They did, however, point out that there may be a sub-group of patients with GT that are more likely to benefit from the targeted gluteal loading used in the GLoBE programme. So does that answer the question then, is education more important than targeted loading in post-menopausal women with GT? It appears it may be for some, especially when you take into account the findings from Plinsinga et al’s work (which we discuss HERE) that found psychological factors, not hip abduction strength were associated with severity in GT. However, the findings from the subgroups and the fact that nearly half the cohort in this study failed to show significant improvement in pain would question the effectiveness of education as a stand-alone treatment.
There are also limitations to this study that may influence how we interpret the results. I believe the largest amongst them is the design of the GLoBE programme and that it may not differ enough from the sham exercises to see a significant difference in the outcome. As the dosage was reportedly the same the exercise load, intensity or specificity would need to be significantly different to see different results. The ‘General to Specific Model’ (below) suggests that weaker individuals will respond to a lower, non-specific strength stimulus. It may be that this post-menopausal population with GT and an average age of around 62 will have been deconditioned enough that even the light stimulus from the sham exercise intervention was enough to increase strength and have a treatment effect.
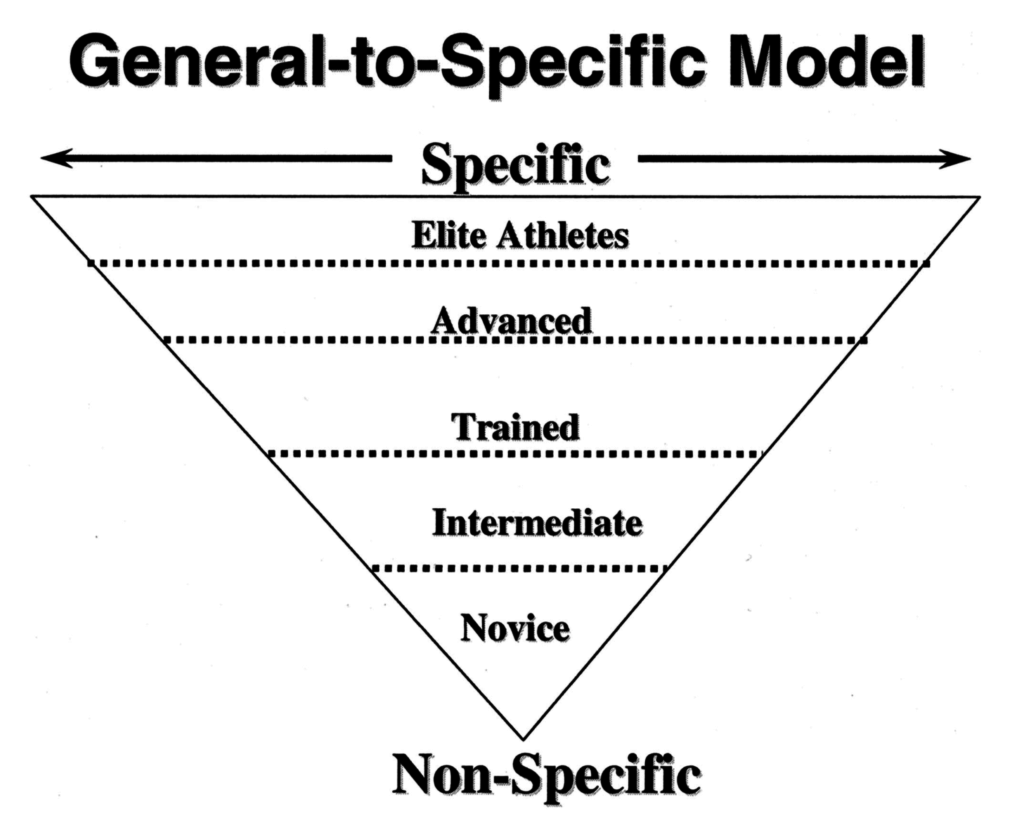
Source: Kraemer and Ratamess (2004)
It is also slightly surprising that there are no exercises in the GLoBE programme working into hip abduction (one of the glute’s main functions) or utilising external load. Studies in achilles and patellar tendinopathy have found Heavy Slow Resistance training to be effective (Beyer et al. 2015, Kongsgaard et al. 2009) and that load magnitude is key in tendon adaptation (Bohm et al. 2015). They’ve also tended to use 3 or 4 exercises to specifically load the muscle and tendon. While the hip hitch exercise has been found to activate the glutes in this population is it sufficient as arguably the only exercise within the programme designed to selectively load the gluteal muscles? A 2016 systematic review highlighted a range of exercise options with moderate, high and very high levels of Gluteus Medius activation. Perhaps some of these could have been included and adapted to suit the needs of patients in this study and ensure more targeted gluteal loading.

Source: Adapted from Reiman et al. (2012)
Limitations aside we do need to recognise that this study included a very different population to those typically included research in exercise prescription and lower limb tendinopathy. This may have proved a barrier for a more challenging approach. In fact, the study mentioned that only half of the participants in the GLoBE group progressed to the end of the program by 12 weeks. Further time with rehab may improve outcomes and allow progression to higher loading within the exercises.
Closing thoughts: This interesting new selection of studies in gluteal tendinopathy is helping to improve our knowledge in this previously under-researched topic. Taken together there are 4 key points I would take from the recent research;
- Gluteal tendinopathy can have a significant impact on people’s lives both physically and psychologically.
- Progressive exercise does appear to be effective for gluteal tendinopathy, with significant improvement seen by around 8 weeks.
- Psychological factors such as depression and pain catastrophizing may be important and questions about mood, mental wellbeing and attitudes towards pain should form part of our assessment.
- Education on activity modification to reduce provocative tendon compression should be included within our treatment of patients with gluteal tendinopathy.
Interested to learn more on Gluteal Tendinopathy? Check out the rest of the series HERE.
We also have a podcast coming out on the topic with the brilliant Karen Litzy so keep an ear out for that!