Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
Following our article on managing acute calf tears we’ve had a lot of questions on swelling and risk of DVT. So I thought I’d clarify a few issues surrounding this with help from 2 excellent physios who have lots of experience of calf injuries through their time working in A & E – Richard Norris and Seth O’Neill. They kindly shared their knowledge on this topic which I have edited into an article. If you’d like to see Richard or Seth for an appointment follow their links above.
Swelling after calf injury
The most common question we receive on RunningPhysio relates to ongoing swelling following a calf tear. Firstly let’s be clear, if you have any concerns after an injury you should consult your GP or Physio for proper assessment and treatment.
While people are often concerned about swelling, it is a normal part of the healing process in this and many injuries. With a calf tear there are several issues which seem to increase the swelling in this particular injury;
- Gravity – your calf and ankle are nearly always below the rest of your body. Swelling simply travels downward and collects in this area.
- Lack of calf pumping mechanism – it is thought that the calf helps to ‘pump’ swelling from the foot and ankle up the leg into the lymphatic system where it can be disposed of. This pumping mechanism happens when the calf muscle contracts and relaxes during activity. When you’ve injured the calf itself working the muscle is often painful and so this normal pumping action is reduced, meaning swelling remains in the calf, foot and ankle.
- Inactivity – after a calf injury it can be hard to walk and remain active. Normal movement helps to clear swelling, so oedema can be aggravated by periods of inactivity.
- The nature of the injury – an injury to a large muscle like the gastrocnemius, which has a good blood supply, can lead to a considerable amount of swelling which can continue for some time as the injury heals.
Muscle injuries take around 6-8 weeks to heal so it isn’t unusual to have swelling that continues throughout this period. In clinic we sometimes see swelling long beyond this initial time scale, it can become chronic and remain for several months. This chronic swelling often presents with ‘pitting oedema’ which can be see clearly over the tibia. Use your thumb to exert a gentle consistent pressure for around 10 seconds then release, with pitting oedema you will usually see a small indentation left in the swelling.

Picture source
Managing swelling
Very important – follow the advice of your Physio or GP!
For acute swelling we generally recommend the following;
- Remain active but pace yourself. Regular small amounts of comfortable activity are usually helpful to reduce swelling but don’t over do it! Too much time on your feet will usually increase swelling
- Elevate the limb when resting – this gives gravity a helping hand!
- Gently bend the ankle up and down to work the calf (with the leg elevated). Little and often is key, recommendations vary so check with your Physio what’s most appropriate for you.
- Ice – there is some debate on whether ice does actually reduce swelling or simply improve pain. More here on ice therapy.
- Compression – a tubigrip or TED stocking can be provided by your Physio or GP. Make sure it’s not too tight and includes the foot and ankle as well as the calf.
- Avoid HARM – Heat Alcohol Re-injury Massage
For chronic swelling (e.g. that has been there for more than 6-8 weeks);
- Elevation, exercising the calf and compression as above
- Try heat to increase blood flow, such as a hot bath
- Massage with the leg elevated can be very effective – your Physio can provide this.
Please note: These are just general guides, specific advice from a health professional is recommended.
Deep Vein Thrombosis (DVT)
A Deep Vein Thrombosis is the formation of a blood clot in a deep vein, usually in the legs. A concern with DVT is that this clot can be mobilised and move to a vulnerable part of the body, such as the lungs, where it restricts blood flow and causes lasting damage.
Astute readers amongst you will have noticed I’m being particularly careful with advising proper assessment from a trained health professional. There’s a good reason for this – my priority is always your health and wellbeing and I don’t want to give out any advice that could compromise this. With calf tears there is a risk of DVT, which, although small, means I don’t want to take any chances by giving out unsafe advice. Please, if you have any concerns don’t scour the internet for answers, see a health professional! A DVT only effects around 1 in 1000 people per year but can have serious consequences, most notably pulmonary embolism, which can be life threatening.
If you have any suspicion of DVT get it checked out by a qualified health professional immediately. In many cases it will be necessary to attend Accident and Emergency.
Diagnosis of DVT is based on signs and symptoms, risk factors and investigations;
Signs and symptoms
- Pain and swelling in the calf
- Changes to skin colour and temperature
- Vein distension
Picture source
Picture source
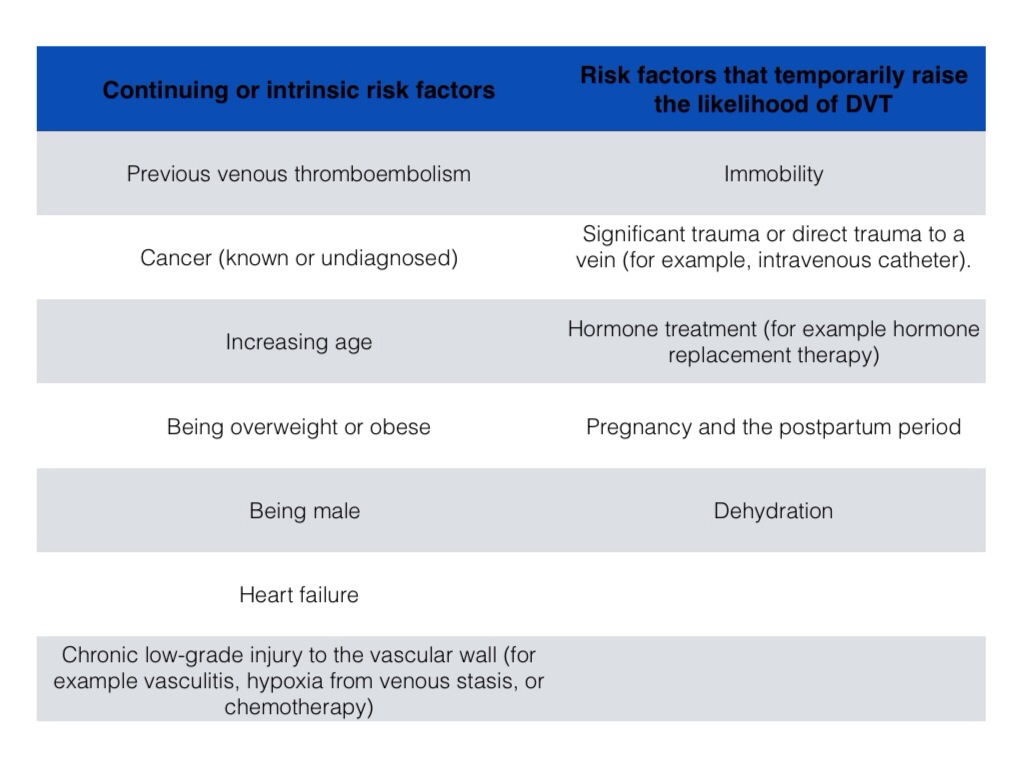
Risk factors
A DVT is considered more likely if signs and symptoms present with known risk factors;
Adapted from National Institue of Clinical Excellent (NICE) Clinical Knowledge Summary;
Investigations
There are two main forms of investigation that are used in diagnosing DVT;
- Ultrasound scan (of the proximal veins of the leg)
- D-dimer – blood test
An assessment tool called the Well’s Score can be used to determine the likelihood of a DVT and guide further investigation and management. This is a combination of signs, symptoms and risk factors;

Reproduced from Scarvelis and Wells (2006) – an excellent article on DVT diagnosis and treatment freely available online.
Closing thoughts: calf swelling is a common and often totally normal part of the healing process following a calf injury and will resolve in time. In some situations where other symptoms and risk factors are present there is the possibility of deep vein thrombosis. This is a serious condition with potentially life threatening consequences. Calf swelling with no redness, or pain, without any risk factors makes DVT less likely especially if the Well’s Score is below 2. Despite this if there is any doubt seek urgent medical advice.












Great article! Thank you!
I believe this is what my husband (age 51) experienced about a week ago. He just started running a year ago and has been very successful. He even lost over 60 pounds. He ran cross country in high school. He wants to run his first 10 mile race on Aug. 10. I have a feeling this is a bad idea as it is too soon after his injury. I also think he should see a doctor to rule out DVT. Any thoughts?
[…] in the British Journal of Sports Medicine blog. Since then Rich has helped out with an article on calf swelling and DVTs and written for The Sports Physio. Today's piece is on ACL injuries and their […]
Do you have consern with the use of compression calf sleeves vs socks as it relates to this post?
My right calf has been swollen for 4weeks now I went the hospitality was 5 cm bigger than left (still is) they ruled out DVD but I’m still getting pain in my right calf and thigh it worries me it hasn’t went down yet what could this be n how long will it be swollen for
Thank you for both articles, Tom, the calf injury one followed by the DVT one.
My mother has just gone into a care home, she loves it, leaving me free after 5 years to live my own life. Imagine my shock when I plumped myself down on the (lowish) sofa and I felt a nasty pain or tension/pull in the area of my kneecap. I straightened my leg immediately in response to the odd pain, and it wore off completely. For the next two days I felt crampy pains in my knee, my thigh, the front of my calf and then the back of it. I read your first article and determined I had better check with GP re DVT, but as it stands he is away for a couple of days…….. Now two more days on, the back of my calf really hurts, in fact it hurts more and more, but the trigger for the pain seems to be when I bend it. No pain on walking, or standing, but going up and down stairs feels “wrong” and often sitting down, so my knee is bent, causes strong feelings of deep inner pain in centre back of calf. I see no cause for worry on Wells Scale you gave us (my diagnosis), I will to to GP asap, but in the meantime, what on earth is going on???? This hurts more and more, and I find it very painful indeed now to get up off the floor, as an example. HARM treatment makes me cringe as I never react well to cold. Also this has happened at the start of colder weather here in France where I live. There are some language issues with GP, his French is better than mine, and I just want to know I don’t have DVT and how to get better. Sorry to be a wimp. Thanks for the outstanding advice Tom. Regards, Claire
Two day ago I was playing basketball when I felt a pop in my calf muscle and I collapsed to the ground in extreme pain. Today I noticed the front side of my leg is swollen. I am worried about a blood clot due to the fact I had knee surgery on 3/14/14.
I heard a pop in my calf about a week ago its swole up felt better then I got a scratch on the front by the shin and it got infected and my whole cast on my leg and my ankle swoll up
My wife had a calf injury, complete with popping sound, in an exercise class a couple of weeks ago. Bruising didn’t show up until a week later. After standing at a trade show all weekend, her foot was quite swollen the other night. Yesterday morning, she had pitting edema and we went to the hospital. Ultrasound/blood tests revealed no clotting. Bruising still there, swelling still there, although ice helped last night. This morning, still swollen, but not as badly. She’s been worried about walking around on it, but I found this article this morning and it made both of us feel a lot better. Now we know that she might be dealing with this for weeks while it heals.
Thanks for the article. Very informative.
Comments are closed.