Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
Tendon problems are common in runners and can become a persistent issue if not properly treated. In recent years our understanding of the pathology of tendinopathy has grown – we now know that it isn’t really an inflammatory process and that load plays a large role. We also know that it’s important to determine the ‘stage’ of the tendinopathy and this will have a huge influence on how you manage it.
Jill Cook and Craig Purdam have been at the forefront of tendinopathy research for some years. Their 2009 paper outlined a model that describes 3 different stages of tendinopathy reactive tendinopathy, tendon dysrepair and degenerative tendinopathy. It is helpful to think of these as a ‘continuum’ rather than 3 completely distinct phases.
Reactive tendinopathy typically involves the tendon responding to a rapid increase in loading. For runners, this often means a large increase in mileage, a reduction of rest days or a change in training type (e.g. Introducing hill or speed work). It can also be from direct trauma to a tendon. It was thought that this reaction involved inflammation but we now understand that this is not the case. The tendon does swell but this is due to the movement of water into the tendon matrix* and not inflammatory products. A key feature of a reactive tendon is that structurally it remains intact and there is minimal change in collagen integrity. Cutting the jargon for mo means this is usually a reversible process. Cook and Purdam (2009) describe it as,
“A short term adaptation to overload that thickens the tendon, reduces stress and increases stiffness”
Tendon dysrepair is usually the stage that would follow reactive tendinopathy if the tendon continues to be excessively loaded. It is similar to the reactive stage but the tendon structure begins to change with greater matrix breakdown. There may be an increase in vascularity and neuronal ingrowth.
Degenerative tendinopathy is more common in older athletes. It represents a response of the tendon to chronic overloading. There are multiple tendon structure changes making it less efficient at dealing with load. Collagen becomes disorganised and advanced matrix breakdown takes place alongside further increases in vascularity and neuronal ingrowth. The tendon can appear thickened and nodular and there is a risk of tendon rupture with advanced degeneration.
*tendons are made up of fibrillar collagen embedded in an extracellular matrix – tendon structure is complex – for more information please see Magnusson, Langberg and Kjaer (2010).
Management of tendinopathy
Cook and Purdam simplify the management by dividing tendinopathy into 2 stages;
- Reactive/ early dysrepair
- Late dysrepair/ degenerative
The treatment varies considerably between these stages. Many runners will have heard of “eccentric” exercise for tendon problems and maybe trying ‘heel drops’ for Achilles tendinopathy or other eccentric exercises. This will probably make things worse in a reactive tendinopathy but might help in the degenerative stage – this is why staging is so important! If you don’t identify the correct stage you could well be making your problem worse!
Managing tendinopathy in the reactive/ early dysrepair phase
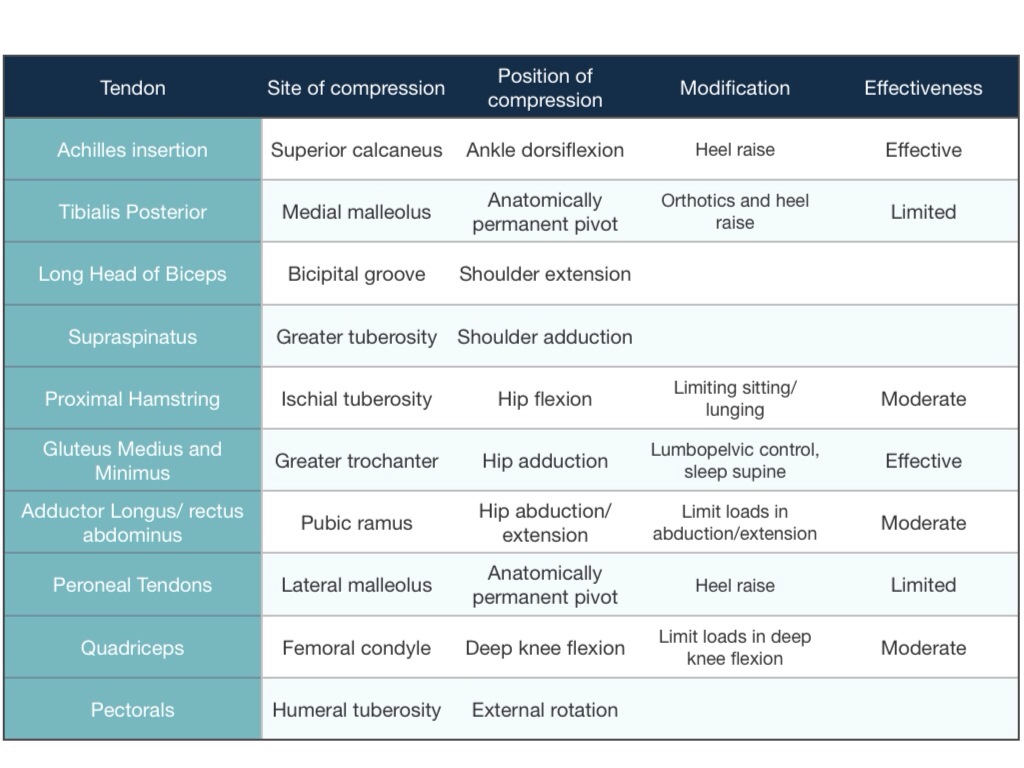
Arguably the most important treatment in this stage is load management. This means reducing both tensile and compressive load on the tendon. Tendons connect muscle to bone and as a result are placed under a great deal of tension during activities that involve the muscle contracting or resisting a stretching force. This is what we mean by tensile load. Each time your foot contacts the ground during running your body has to deal with an impact force equal to roughly 2.5 times your body weight. Fortunately, tendons are thought to be able to withstand up to approximately 8 times our body weight. Runners can reduce tensile load simply by decreasing how far or fast we run or taking a rest from running if indicated. However, tendinopathy often has a compressive element to it that also needs to be addressed. For example, with proximal hamstring tendinopathy, the tendon is thought to be compressed against the ischial tuberosity (bone in your bottom) when the hip is flexed, such as during sitting. Reducing time spent sat is a simple way to reduce this compressive load. Of particular importance is reducing movements that combine both compressive and tensile loads. Staying with the example of hamstring tendinopathy, running uphill and stretching the hamstring muscle can both place tension on the hamstring while it’s tendon is compressed against the ischial tuberosity. As such both are likely to aggravate the condition, especially in the reactive stage.
Cook and Purdam (2012) describes the potential role of compression in tendinopathy. The following is adapted from some of their findings in that paper;
Managing load doesn’t mean completely offloading the tendon (I.e. by hopping around on crutches) but reducing the load to a level that allows the tendon to recover. This may mean rest from running or modifying training depending on the severity of tendinopathy. The reactive stage can be relatively short – Jill Cook talks about this in her excellent podcast (on PhysioEdge) and says pain may settle in 5 to 10 days but the tendon will still be sensitive to high loads and training needs to be progressed gradually to prevent relapse. When managing load be guided by how the tendon responds not just immediately but also 24 hours later. Tendons are known to have a latent response to loading. This means they can take 24 hours or more to react to it. Bear this in mind when running – it may feel fine at the time but react the next day.
Despite the lack of inflammation anti-inflammatory medication is thought to be helpful in the reactive stage. This is thought to be because it inhibits the production of proteins responsible for tendon swelling. Ibuprofen is considered one of the best drugs for this role and is not thought to have a detrimental effect on tendon repair. That said, while Cook and Purdam favour the use of these medications in the reactive stage Karim Khan is far less positive in his podcast on achilles tendinopathy. Green tea is also thought to be helpful as it contains an anti-oxidant called EGCG. Always consult your GP or pharmacist before taking medications.
Isometric exercise can reduce pain and maintain muscle strength in the reactive stage (provided it’s not done in a position where the tendon is compressed). We’re hoping to add a specific article on this soon. Isometric exercise is where the muscle works against resistance without creating joint movement or changing muscle length. Let’s try this with a facepalm! Place the palm of your hand on your forehead. Push your head forward into you hand but keep you hand still. Your neck muscles are working but your head isn’t moving so they’re working isometrically. The educational power of a facepalm!…
Silliness aside I hope this illustrates what isometric exercise is – work the muscle without movement. Specific isometric exercises will be discussed for each particular tendon in individual articles. I recommend asking your physio to show you exercises specific to your case. Below is an example of an isometric quadriceps contraction from Sportsinjuryclinic;
Don’t stretch – now this might promote some debate amongst runners and physios but in many cases it’s sensible not to stretch a reactive tendinopathy. Often we want to throw everything at an injury to make it better but sometimes it’s best to stick to what we know works. The issue with stretching is the potential for tendon compression. The hamstring tendon, for example, is often compressed during stretching which is likely to aggravate symptoms. Sometimes muscle length is an issue you need to address but it is probably wiser to do this after the reactive stage. You might find using a foam roller or trigger ball can help improve flexibility without causing tendon compression. Allison Grimaldi talks about this on her brilliant podcast on hamstring tendinopathy. However, I would work the main bulk of the muscle and avoid pressure over the tendon area. Cook and Purdam (2012) suggest massage may be a better option than stretching to manage muscle length and flexibility in compressive tendinopathy.
Run or rest? The temptation to kit up and hit the road is always there as a runner, sometimes though it is important to allow adequate rest first. Reactive tendinopathy is often one of these times. Choosing to run or rest is actually quite a complex decision. A host of factors play a part – are you training for a race or just training in your off-season? How severe and irritable are the symptoms? Can you find a way to run without pain (both at the time and 24-48 hours later)? How is your body generally – are you struggling with a host of niggles that need some rest? What is the bigger picture here – will timely rest now stop this from becoming a persistent, long term issue? I think with tendinopathy it’s best to air on the side of caution, especially in the reactive stage. We know load management is arguably the most important part of treatment so if you continue to load a reactive tendon it may stay in that painful reactive stage or progress to include structural changes within the tendon. It’s a bit of a balancing act though, as offloading the tendon for too long is also unlikely to be helpful and many physios will advise to continue some level of running if possible.
As a very general guide, I would suggest you want to be fairly comfortable both at rest and walking before starting running again. Try jogging on the spot too and see how that feels. The best guide though is to see a qualified health professional and take their advice. They can give you the green light to begin running again with the benefit of a full assessment, something that sadly we can’t offer through online advice!
When you do return start with a short distance or even a run-walk pattern and see how it feels. Resist the temptation to increase distance on that first run if it feels ok. See how it responds over the next 24-48 hours and go from there. When you run may also play a part – sometimes tendinopathy is worse at certain times of the day, often people complain of more pain in the morning for example. It may be wiser to run later in the day if the tendon is less sensitive then.
The good news though is you can often cross-train as long as you choose exercises with little tensile or compressive load on the tendon such as swimming, cycling or comfortable gym work – again be guided by symptoms during and after exercise.
Late dysrepair/ degenerative tendinopathy
This tends to be more common in the older athlete although can present in younger runners with a history of chronically overloading the tendon. To confuse matters somewhat you can also have reactive tendinopathy alongside degenerative. This is because parts of the tendon may become degenerate while other parts remain fairly normal. The ‘normal’ non-degenerate areas of the tendon can respond like any other tendon to excess load and enter a reactive stage. If you have had a grumbling tendon for some time, the tendon is thickened and has palpable ‘nodules’ within it then it’s likely you have a degenerated tendon. If alongside this you’ve suddenly had an increase in pain in response to increased mileage you may well have reactive tendinopathy alongside a more chronic degenerate one. If this is the case the principles of managing a reactive tendon apply – manage load, consider anti-inflams and use isometrics until things settle.
For your more chronic, grumbling tendon without a sudden increase in pain, a mixture of load management, eccentric work, isometrics and strength exercises are likely to help. Some of the changes within the tendon may be reversible but it is likely this is a condition that will need to be managed in the long term.
Load management – a key here is know what aggravates your symptoms. When you know what makes things worse then you can focus specifically on changing that. There are two parts to this theory and practice. Know the theory and see what happens in practice. For example proximal hamstring tendinopathy;
- Theory – symptoms will be aggravated by compression of the tendon such as sitting on firm surfaces, stretching the hamstring, leaning forward with the knees straight and by high tensile load such as running fast, over-striding when running or carrying a heavy load (e.g. Running with backpack). Running uphill is thought to combine both compression and tensile load and is especially provocative.
- Practice – make a note of what actually aggravates your symptoms as you may not fit the textbook! A training diary is very useful for this. Note what running you’ve done and any symptoms each day and this might give you a better idea of what to change.
- Management – avoid hills and speed work initially. Stick to a comfortable pace with smaller stride length. Gradually re-introduce potential aggravating factors but allow the hamstring tendon time to adapt and monitor symptoms.
Rest – a big part of managing tendinopathy is how you use rest. Tendons can adapt to load given adequate rest time. This process takes around 3 days following exercise but you may find just allowing 1 rest day between runs is enough to prevent repeated tendon overload. For those of you running 5 or 6 days a week a rest day after your long run may be more beneficial than a ‘recovery run’. If you have a degenerate tendon it might be sensible to replace 1 or 2 of these runs with rest or cross-training.
Graded increase in mileage or training intensity – in order to allow the tendon to adapt to load, changes to training need to be done gradually while monitoring symptoms. Change one thing at a time and plan enough rest after!
Eccentric training – it’s generally accepted that eccentric training is a useful part of managing degenerative tendinopathy. However exactly how you do this will vary greatly between individuals. There is no recipe here I’m afraid! Strength, power or endurance work will also have a role and help in preventing problems in future. Identify any biomechanical issues that may place additional load on a problem tendon as they may need to be addressed to prevent relapse with increase mileage.
Further details of training regimes and how to identify potential causes of tendinopathy will be discussed in more detail in each individual tendon article.
Final summary: staging tendinopathy is important to guide management. Cook and Purdam (2009) describe it in a nutshell,
“An older person with a thick nodular tendon is likely to have a degenerative tendon; conversely, a young athlete after acute overload with a fusiform swelling of the tendon will probably have a reactive tendinopathy”
As ever on RunningPhysio we recommend assessment from a qualified health care professional to help you manage what can be a persistent and difficult injury.
If in doubt get checked out!











[…] Tendinopathy is usually divided into stages. Initially you have a reactive stage. This is usually a response to rapid increase in loading. The tendon may visibly swell and will be painful. In more chronic cases there is often a more degenerate tendinopathy and the tendon's structure is changed considerably – it may be thickened and develop nodules. If untreated the degeneration of the tendon can reach a level where it really can't handle any load, as a result it fails and you develop a partial or total Achilles tendon rupture. This is a gradual process and usually a painful one but sometimes it can occur without pain with the first sign of a tendon problem being a sudden unexpected rupture. Working out the stage of the condition is important to determine the best treatment – see our article on staging tendinopathy. […]
Thanks for your great article. I am suffering with tendinitis at the moment, it’s my extensor tendon which leads to the big toe which is the problem. I’ve had it 3 weeks, during which time I have rested from running, but it’s no better. I’m seeing a physio, but I wondered if you knew what might compress foot extensor tendons? I’ve been stretching the top of my foot by kneeling on it, maybe this could be aggrevating? Also I have been cross training with spinning, but I’m wondering, after reading this, whether the baskets on the spinning bike might aggravate the tendon by pressing on the top of my foot. Your thoughts would be much appreciated.
Hi Rebecca,
Sometimes old or ill fitting shoes can compress the tendon. Worth making sure the shoe feels comfortable in the toe area. Sometimes the sole of the shoe loses it’s rigidity and starts to bend excessively at the toe section – I’d check that too.
I think I would stretch the calf muscles rather than your toe extensors – a tight calf is thought to increase great toe extensor activity which can cause the problem.
Spinning may be a factor too – the only way to know is to see how your symptoms are during spinning and the day or so after. If there is no increase in pain it’s probably fine.
Hope that helps
Tom
Hi, yes it does help, thanks. I was running in old shoes before it happened, I hadn’t thought about the flexibility of the sole. It’s hard to tell with the spinning, the pain goes up and down and doesn’t seem to be related to anything in particular!
[…] ← Previous […]
Hi Tom
Another great, well written and researched article, I do like your work pal! I’m really pleased you have included the use of isometrics as a treatment in a reactive tendinopathy as I think this is a really under utilised treatment that most physios think are only suitable for post op knee replacements.
HOWEVER… (there’s always a however isn’t there) just one small little minuscule thing!
I don’t think the demos you have included for quad isometrics for patella tendinopathy are suitable for a number of reasons, first its in a non weight bearing position so no matter how hard you squeeze there just won’t be enough load on the patella tendon to generate the therapeutic force needed in the tendon, secondly its not in the right position ie full extension, the knee should be positioned so that the patella tendon is maximally loaded around i’d say about 30 degrees flexion and lastly they are just not held long enough for a therapeutic effect, should be a minimum of 5+ seconds.
We know that isometrics apply an actual eccentric lengthening force on the tendon unit as the muscle unit contracts but without any combined total change in whole musculotendionous unit length thanks to Farris et al (2013) paper, and although still to be fully researched the EIS and most other including me, recommend that isometrics are done Heavy (ie 80%+ body weight) slow 5+ secs and frequent 3×10 3x a week.
I would suggest a single leg quad dip and hold for patella tendinopathy’s even holding extra weight or in a rucksack, or done on a leg press on a machine in 30 degrees flexion with heavy weight on and get the single leg to hold the weight, for Achilles same as a heel drop position but just without the drop.
Hope that helps mate, great work again
Cheers
Adam
Hi Adam,
Thanks for your comments, very helpful as ever!
I agree with you 100%!
The isometric quads exercise I included is just an example of an isometric exercise rather than what I would recommend for patella tendinopathy. You’re right that a single leg squat (usually done on a 25° decline board) is more appropriate and recommended by Gaida and Cook in their 2011 review.
I was just trying to demonstrate to non-medic types what an isometric contraction looks like!
I’m working on a patella tendinopathy article at the mo with specific advice for that condition.
Cheers
Tom
Tom & Adam
I am an MSc physiotherapy student and came across Tom’s article and your discussion, whilst trying to get some background knowledge on the role of isometrics in tendionpathies – a potential dissertation topic!
Tom, your article states isometrics reduce pain and improve muscle strength however I was wondering if this was based on your clinical experience or whether these are evidence based claims?
Adam, you helped shed some light on volume and exercise prescriptions however I had the same query?
My problem being I can’t seem to find any literature into the role of isometric exercise in the treatment of tendionpathies. I was wondering if either of you would be so kind as to direct me towards any sources that supported your work or authors in this field?
Any help would be greatly appreciated.
James
Hi James!
I would look at some of the work of the tendon gurus like Pete Malliaras, Karen Silbernagel, Jill Cook to start with, think Pete looked at different treatment protocols recently in a paper so might have more info on isometrics there.
Also follow a guy on Twitter called @fizziowizzio he is a wealth of knowledge on tendons, has bad banter but can’t have everything though hey!!!
Good luck
Adam
PS with a surname like yours I have to ask, are you related to my old boss at Watford FC Richard Collinge!!!
Thanks Adam,
Excellent input as ever!
James,
I’d add the work of Keitaro Kubo to what Adam suggested – he’s widely published in tendinopathy and response to exercise.
There are links to lots of tendon info on our Physio Resource Page
Thanks
Tom
Brilliant! Thanks for your help lads.
If only, no relation I’m afraid Adam!
[…] Cook and Purdam (2009) highlighted the importance of determining the ‘stage’ of a tendinopathy in determining management. They suggested that clinically 2 broad stages could be used – reactive/ early dysrepair and degenerative/ later dysrepair. In the reactive stage the tendon responds to excessive load by thickening and stiffening which helps act as a stress shield to decrease load. Unfortunately this process usually results in pain but is reversible and settles when the excessive load is removed. In degeneration the tendon structure changes and there is change in the collagen which makes up the tendon. For more on this read staging of tendinopathy. […]
Very interesting article. I have been trying to find something online about my specific problem I have been dealing with for a while. In doing alot of research, I am feeling them my Extensor Tendons on top of foot are possibly experiencing Tendonitis. I have been a runner for 3 1/2 yrs now. I am 45 yr old female. I have ran 4 Half Marathons (road) and 1 Trail Half. I am YET TO COMPLETE them without cramping and feeling it in my toes, bottom of foot sometimes, calves, and ankle just feels “tight”. It constantly feels twitchy, even now that I am not running. Here are a list of symptoms…. waking up with night cramps with hammertoes, contstant tightness around the top part of my ankle/foot on the tendon that I can determine is the Extensor Digitorum Longus, because it does affect my four toes, the tendons that run over my ankle on the Dorsal side. – This past Saturday, I ran the Trail Half and actually it felt pretty good until the last 9 miles as that is always the time it will start flaring up. When I finished I went to get it massaged, but could not even make it through the session because it was flaring up so bad. He would work on the calf some and it would release, but then the foot would flex up and the toes would cramp. He stated that he could see the Tendon flared up on top of the foot and I needed some Active Release Technique, which is what they do at his Chiropractic office. He would Stretch it out by pushing my foot down and inward, plus at the same time he would Rub upward which felt good in a sore kind of way…. He said I definetly had those tendons flared up.— Back in December, I did a Half that had MANY HILLS… and at mile 10 I had the major cramp in this calf…it was like a rock…. pretty much took 4 days to even walk right. I am now thinking that is what flared up that stuff down there. Ever since then it seems tight when I run…like I cannot move the foot freely. Any Advice??? Does this sound like something you have experienced?
[…] – reactive (and early dyrepair) and degenerative (and late dysrepair). More here on staging of tendinopathy. I discussed staging of gluteal tendinopathy with Alison Grimaldi and she said it's easier to […]
Hi mate,
Excellent article as always. Being an Australian, the work of Jill Cook & Craig Purdam has been revolutionary in our profession – once again the Aussies leading the way (just like the Ashes later this year hopefully! 😉 ).
Just a note on what I commonly see in clinical practice – too many Physiotherapists neglect the role of compression in Tendinopathy and I am very glad you have brought this up. Numerous times I have had patients come to me with chronic proximal hamstring tendinopathies that have been prescribed squats/single-leg squats (presumably in the aim of improving posterior chain strength and lumbopelvic control) without consideration of the role of compression. These people commonly say their aggravators are prolonged sitting, yet they are given squats as an exercise and wonder why they aren’t improving. I agree squats are an excellent exercise and probably what I prescribe most due to it’s functionality, however consideration must be given to the compressive force that a squat will place on that proximal hamstring insertion. As you have already stated, start with the isometrics and then progress on as their symptoms reduce.
Keep up the good work!
Hi Justin,
I have hamstring tendinopathy and have just moved from isometric exercises to eccentric. It flared up the day after and I have tweaked it a few times since leaving it sore and more consistent pain. Should I expect to progress through the different stages of rehab pain free? Isometrics were fine but the eccentric seemed a little too much for it. If it flares up is a rest day between exercises ok? Thanks.
[…] tackling this piece on rehab I recommend you read our article on tendinopathy staging and compression as this is the foundation for much of the work […]
Are there any foods, supplements, over the counter or prescription medications that are helpful for degenerative tendinopathy?
[…] Tendinopathy […]
[…] 3. Blog Tom Goom: Blogpost Tendinopathy – the importance of staging and role of compression […]
Good article ! I’m an aging hockey player diagnosed with degenerative high hamstring tendinopathy a year ago. After 6 months off, lots of stretching and eccentric strengthening, I’m back playing and training fully, but a weekend of 2 really tough games have aggravated it again. A lot of sitting at work and driving doesn’t help either. My question – the eccentric exercises are single leg pillars with a 2kg weight. These help, but are they best done before I play, after I play or on days when I don’t play ?
Physiotherapists in Tralee. Nice little article.Below is a link to a blog on our website on tendinosis, very much in line with the above article overviewing treatments….what to do and what not to do in a simplified manner….I hope it proves informative.
http://www.physiotherapiststralee.ie/tendinosis-treatments/
Comments are closed.