Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
I spent much of my university years staring at people in their pants. It was a big part of our course and we’d spend hours picking over static alignment and deliberating over minor postural differences. For many clinicians, it still represents a big part of their assessment but with so many things we could assess and limited time available is it still of value?
Let’s start with an example…
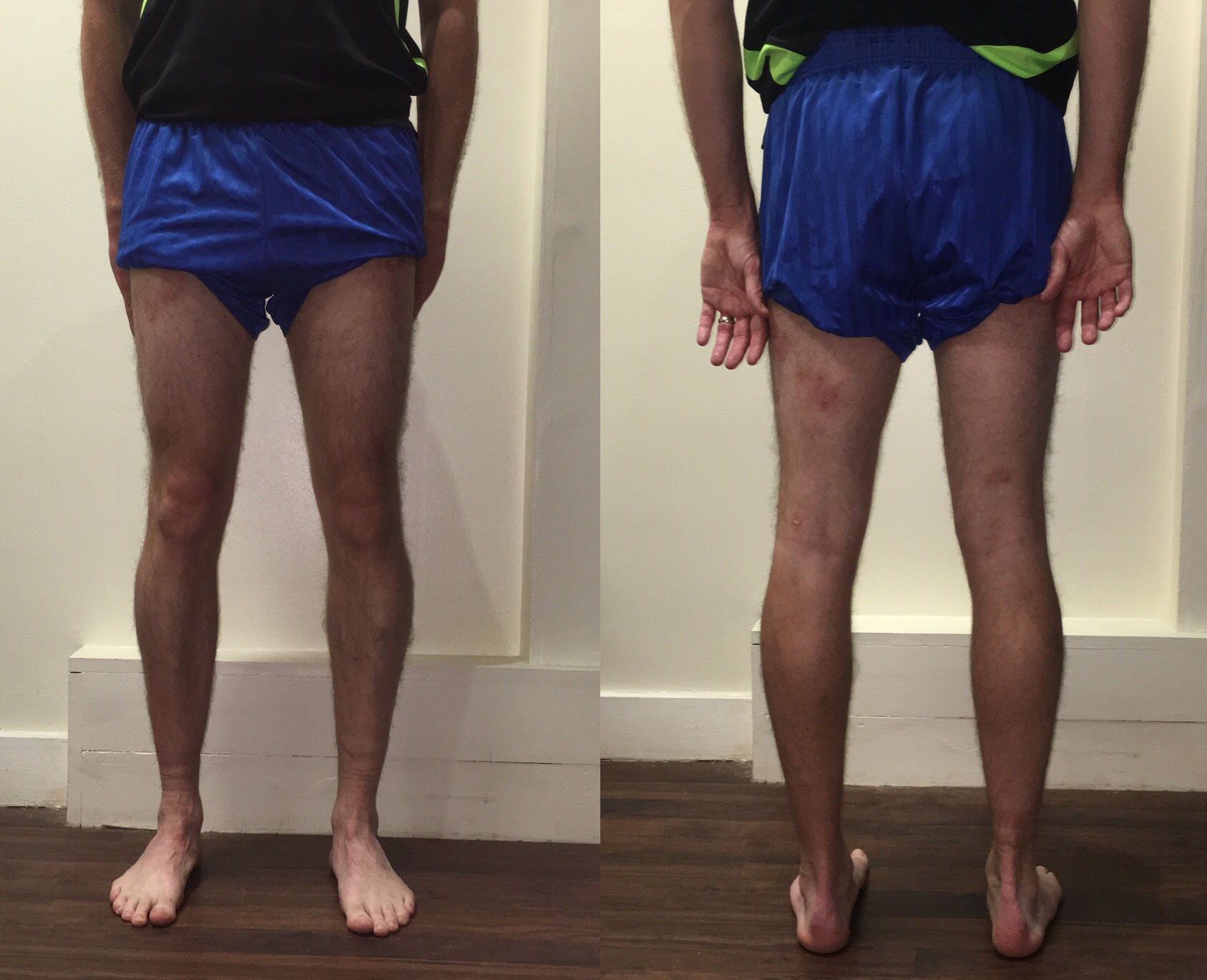
Where do we begin? Well for a start those shorts are dreadful and I can imagine @AdamMeakins asking, “do you even lift bro!?”. They are seriously skinny legs, especially the ankles, but they are my legs and they’ve carried me well over thousands of miles of running!

There’s noticeable genu varum, perhaps more so on the left and a more detailed examination would reveal a 1-2cm leg length difference. At closer inspection, you’d see a slight loss of left quads bulk and some minor swelling over the distal left fibula (which hurts a bit, but only if you prod it!).
I’m sure you could pick out more and spend 20 minutes measuring this, that and the other but is it worth it? Does it really tell you much that helps in managing running injury? The evidence would suggest maybe not…
…let’s start at the pelvis and work down and see what the research says about some of the static alignment variables we might measure.
Hip and pelvis
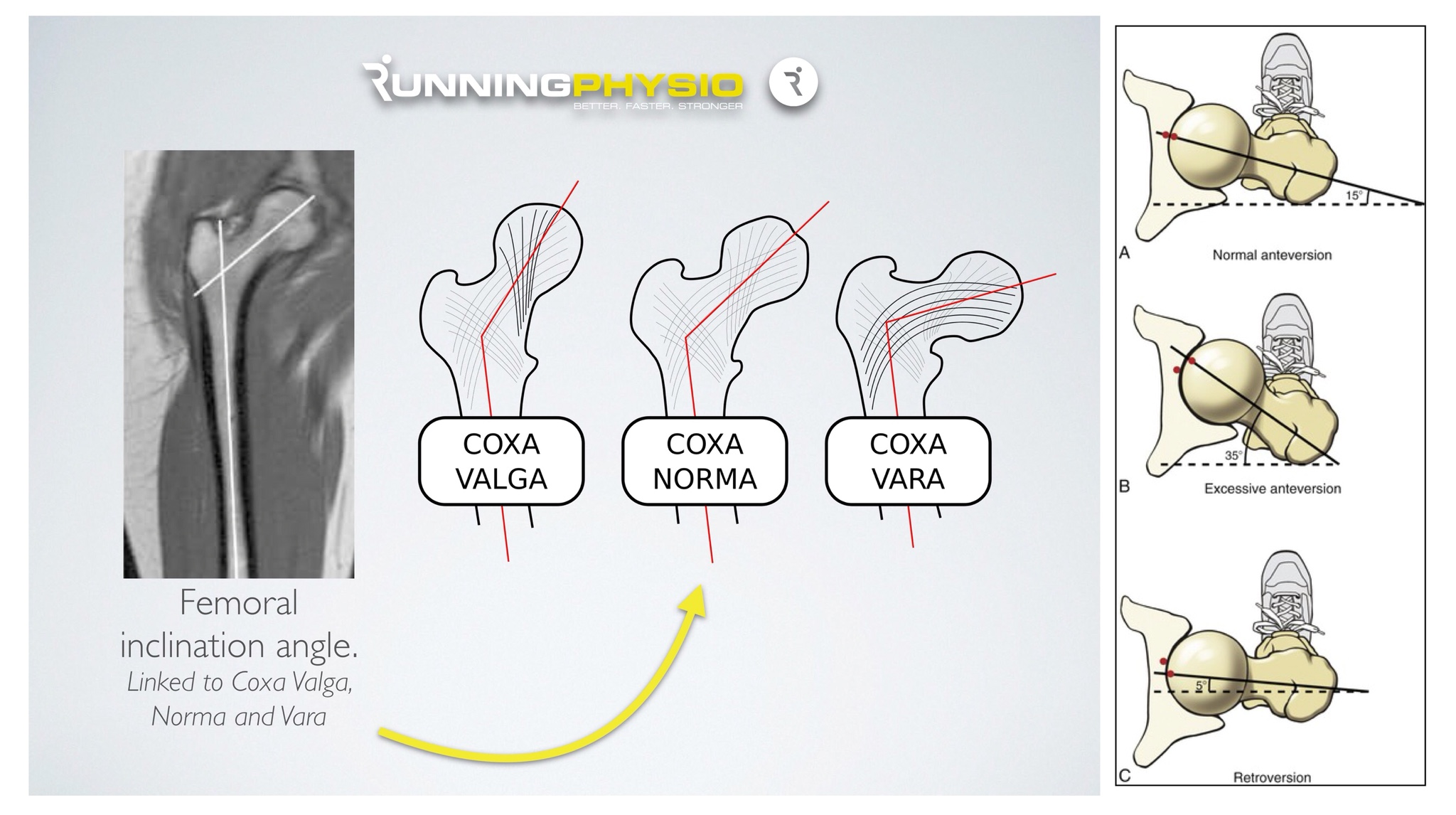
Femoral inclination angle image, adapted from Souza and Powers (2009). Anteversion image source.
A recent prospective study found leg length discrepancy was not associated with running injury in recreational runners (Hespanhol Junior et al. 2016). Souza and Powers (2009) compared muscle performance and anatomical variation (femoral inclination and anteversion) with internal rotation during running in those with PFP and without. They found no difference in hip anterversion between the groups and while the femoral inclination angle was significantly greater in the PFP group, the average difference was just 4.4°. Despite this difference femoral inclination and anteversion were not associated with hip internal rotation during running.
There were significantly differences in muscle performance in 8 out of 10 tests between the PFP and control groups. Of these only hip extension endurance was a significant predictor of hip internal rotation during running. This led the authors to conclude,
“Abnormal hip kinematics in women with patellofemoral pain appears to be the result of diminished hip-muscle performance as opposed to altered femoral structure.” Souza and Powers (2009)
Baggaley et al. (2015) had similar findings with regard to anatomical measurements; femoral inclination angle and pelvis width – femur length ratio were not associated with hip adduction during running.
Knee
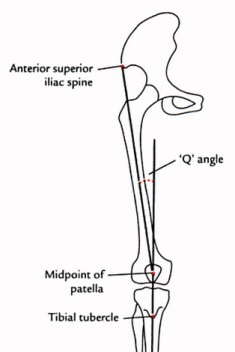
Hespanhol Junior et al. (2016) found that Q-angle was not associated with running injury. This mirrors a previous prospective study by Ramskov et al. (2013) who found that Q-angle did not appear to affect risk of injury in novice runners.
Image source
Foot and ankle
Arguably the most talked about variable here is foot pronation. Conventional wisdom would have us believe that ‘over-pronation’ is the root of all evil. Some sources suggest 70% of people ‘over-pronate’ and this causes a host of injuries.
The evidence in runners doesn’t appear to agree. Ramskov et al. (2013) found static foot posture (measured by foot posture index) did not affect injury risk. Nielsen et al. (2014) performed a 1 year prospective cohort study of over 900 novice runners. They concluded foot pronation was not associated with an increased injury risk. In fact, those classified as having pronated feet sustained significantly fewer injuries per 1000km than those with ‘neutral’ feet. The study points out though, as a limitation, that few runners with ‘highly pronated’ feet were included in the study.
More recently Hespanhol Junior et al. (2016) found subtalar angle and plantar arch index were not associated with running injury. Lun et al. (2004), who measured a number of factors including standing ankle pronation and assessment the longitudinal arch, found that static lower limb alignment did not appear to predict injury in recreational runners. They did note, however, that aligment factors may be injury specific.

Image source
An excellent systematic review by Neal et al. (2014) did identify evidence that pronated foot posture may be a risk factor for Medial Tibial Stress Syndrome and Patellofemoral Pain. This research included 21 studies with varied populations including runners and non-runners. Dowling et al. (2014) did a similar review of dynamic foot function and found very limited evidence that it was a risk factor for patellofemoral pain, Achilles tendinopathy, and non-specific lower limb overuse injuries. They also comment that it’s unclear if we can accurately identify these factors clinically or if they can be modified to help prevent or manage lower limb injury. (Both these papers are Open Access and well worth a read – huge credit to @Brad_Neal_07, @Sports_Pod, @DrChrisBarton and team for their excellent work putting them together)

Limitations
It’s very difficult to provide a definitive answer on the topic of static alignment in runners. The consensus in the literature appears to be that most are not significant risk factors for injury and may not influence running gait as we’d expect. There are however a host of issues that muddy the waters;
- Multiple factors have been measured
- Different techniques are used to measure the same factor (I can think of at least 5 just for pronation!)
- These techniques might be very different from what we have available in clinic (e.g. MRI or CT for hip anteversion)
- Definition of running injury varies and different running populations are examined across the research.
- Most studies don’t examine specific injuries but look at injury risk in general. This can be because of insufficient sample size to enable them to create sufficient episodes of 1 particular injury to study it in detail.
- Research of this type is hard to do. Ideally it requires prospective study of a large number of runners over a long period of time with accurate reporting of injury and training data.
- There are many more variables that I haven’t been able to examine in detail for this blog. I hope to update this article with more information as new evidence emerges.
Conclusions
We must be mindful of the limitations above and resist the temptation to make concrete conclusions on this complex topic. The literature appears to suggest;
- Static lower limb alignment may not correlate with running gait patterns
- In general static alignment does not appear to influence injury risk although some factors may be weakly associated with specific injuries.
- Muscle function may be more closely related to injury risk and running gait, although this connection is complex and strengthening alone doesn’t appear to significantly alter running gait kinematics.
- Static alignment is generally a ‘non-modifiable’ factor. There are a host of modifiable ones such as athlete education, training structure and progression, strength and conditioning and running gait that we could address instead!
I’m certainly not suggesting we abandon static assessment. It may point us to other relevant findings, such as muscle atrophy or swelling. It may also provide useful information about specific injuries, for example acquired flat foot deformity secondary to posterior tibial tendon dysfunction. With limited time available, however, we would perhaps be wise not to spend most of it focussing on static alignment and instead explore more useful parts of the biopyschosocial assessment…
…let’s spend more time getting people moving and less time standing still!










Nice legs Tom!!.. I think we were all schooled in these paradigms, without having adequate emphasis placed on dynamic function, and more importantly dynamic assessment. Pleasingly, this does slowly seem to be changing. From a podiatric perspective, I have not taken a static foot or leg measurement (for example “relaxed or neutral calcaneal stance position) in years. I just cannot see how this is relevant to the injured athlete. And as has been pointed out so well by others.. where is the line in the sand for overpronation anyway? No-one knows.
I think it is way more valuable to strive to reproduce the load that caused the problem, and try to identify the dynamic deficits that may have contributed. Thanks for the piece.. great read as always!
best
Simon
Comments are closed.