Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
If you have back pain please read our guide on acute management first, it forms the basis of all our back pain articles. Our follow up piece on exercises is also designed to complement this post.
The back is a complex thing. What sets it apart from other areas is how many factors can affect it. In our first article on this, we looked at different severities of back pain and then followed it up with some suggestions on rehab. This piece will cover some of the other key points when managing your back.
The back is sensitive but strong
Something we see in back pain that is much less common in other areas is ‘sensitisation’. This is a complex process involving multiple parts of the nervous system with the result being that the back becomes very sensitive to movements that stretch the back or activities that place pressure it. In some cases even lightly touching the back can cause pain. This doesn’t happen with every back problem but for some people, it can mean that even gentle exercise can increase pain.
How this works, without getting too technical, is that the nerve endings within muscles, tendons, ligaments etc become more sensitive so it requires less stretch or pressure for them to fire nerve impulses which will reach the brain and be processed as pain. Not only are these nerve endings more sensitive but their output increases meaning a small stretch or movement can result in a barrage of nerve impulses being sent to the brain. This is represented in the pictures above – on the left is non-sensitive – lifting a weight while bending causes some reaction from nerve endings in the tissues. Impulses are sent to the brain but may even be filtered out along the way so you won’t necessarily feel any pain. The picture on the right is a sensitive system. It only takes the small amount of pressure involved in standing for a few minutes to trigger the nerve endings to send impulses. When it does this, these sensitive nerve endings send loads of impulses (a barrage) and these then reach the brain where they are less likely to be filtered out. The result is likely to be high levels of pain.
In the vast majority of cases, this severe pain exists without tissue damage – it occurs due to sensitivity of the nervous system. In fact, less than 1% of people with back pain will need to have surgical treatment for their symptoms.
So while the back can be sensitive it is a strong, stable structure. It gets its stability from 3 systems – bony stability (the bones lock together like 3D Jigsaw pieces) ligamentous stability (each vertebra is connected to other levels by at least 5 or 6 strong, fibrous ligaments) and muscular stability (a mixture of deep and superficial muscles connect to the spine and surrounding tissue to provide stability during movement). It’s fair to say that the spine also doesn’t ‘slip out of place’ (and nor can it be ‘put back into place’ or ‘realigned’). This is terminology misleading. The muscles on one side can be tight, meaning you tend to lean one way, or the spine can have subtle curves in it but without major trauma, it won’t be ‘out of alignment’.
Key point: the back can become very sensitive, this doesn’t mean damage – the spine is a strong, stable structure.
Pacing
Knowing movement won’t cause damage is helpful but it doesn’t necessarily tell you how to make progress or how to settle a sensitive back. This is where pacing is crucial.
If there is one skill I could teach any patient or any runner it would be to master pacing.
Pacing is doing things at the level you can cope with. It means not pushing through pain and understanding your limits. At its best, it’s modifying activity to reduce pain but to continue to progress…and it works. In time pacing will reduce sensitivity in the nervous system and reduce pain.
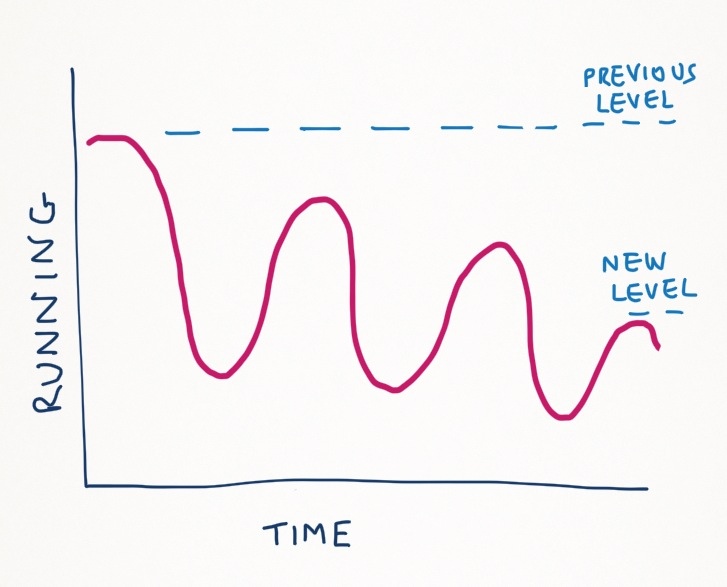
Often if people don’t pace they actually find they can do less and less. For example, you run 2 miles pain-free but at 2.5 miles your pain starts. You continue to 3 miles but it’s getting very uncomfortable. Your schedule says 5 miles so you push on. By 4 miles you have to stop. You’re frustrated and sore. The next few days are a write off in terms of any exercise and it’s a full week before you can begin to run again. This is called boom and bust. You exercise above the level you can cope with (boom) and then your pain gets worse and you rest totally for a week (bust). Your running (or activity in general) starts to do this;
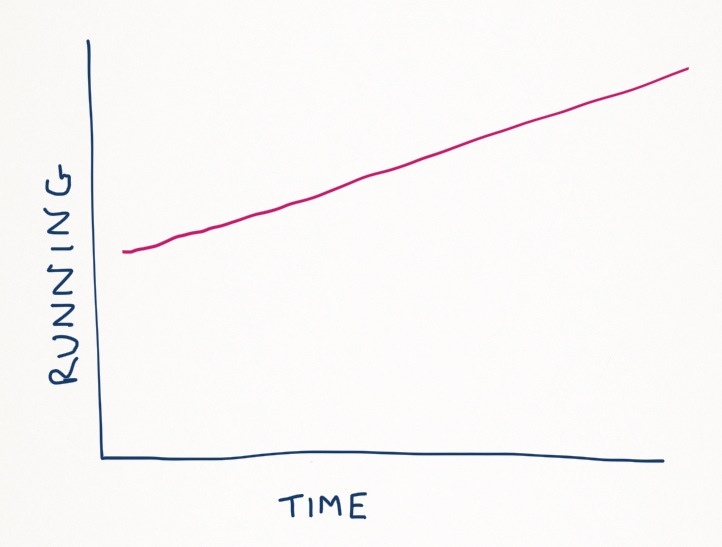
In the example above if you were pacing you’d stop at 2 miles. You may have run half the distance that day but you’d be comfortable and able to run again in a day or so. You could then gradually increase the distance so in time you can achieve your target mileage;
One of the first steps in pacing is finding your baseline this is the amount of an activity you can do without an increase in your symptoms. So, in the example above, the baseline would start at 2 miles. This is something you might need to work out for a number of things that can increase your pain, not just running. It really depends on how severe and irritable your pain is. To work out your running baseline run (on a treadmill if possible) at long run speed (a comfortable speed you can chat at) and stop when your pain starts. Note the distance and time. Now take 10-20% from that. This forms a baseline below the level at which you get pain. For more on using this baseline see our article on returning to running.
For some reading this, running may be some way off you may be finding walking or other activities painful. The same principles apply – find a baseline level that you can comfortably and gradually build up that level. You may even make a pacing chart;
The idea would be to stick to your baseline where possible. Sometimes you may have to overdo it a little (life won’t always follow your pacing plan) but try to pace where you can.
For some this may seem very basic, it depends on your pain. You could just as easily replace those activities with advanced stuff – one for tempo runs, one for intervals, one for hill training – each showing the level you can manage for each that doesn’t flare up your pain. Or you could fill it with each of your exercises – the reps you can manage for each. The extent at which you pace is entirely your choice, it can be something you apply to everything or selectively to 1 or 2 things that really aggravate your pain.
Key point: pacing is the art of doing what you can manage. It is designed to be progressive – in the long term you will gradually work towards your normal levels. Pacing reduces pain and sensitivity, its alternatives are boom and bust or avoidance (just avoiding what hurts) and neither of those will work.
Modify to achieve more
Part of pacing is modifying what you do – it’s not always about doing less. Running has many variables you can change, the obvious ones being speed and distance but also you can change running surface/ terrain, running shoes, how frequently you run and your warm-up and cool down. You can offload using taping techniques or try to alter your running form a little with a shorter stride length or leaning slightly further forward/backwards. See what you can change that helps your running. It’s a case of trial and error. This technique is really useful with most running injuries – I’ve had knee issues (as some of you may have read in previous posts). I found running a little slower and reducing my stride meant I could significantly increase my distance. See what you can change that gives you a bigger baseline.
The same applies to any activity that aggravates, see what you can change. If it’s cycling that hurts try adjusting your seat height or cycling in an easier gear. If its exercises change the reps or how far you push them.
Deconditioning
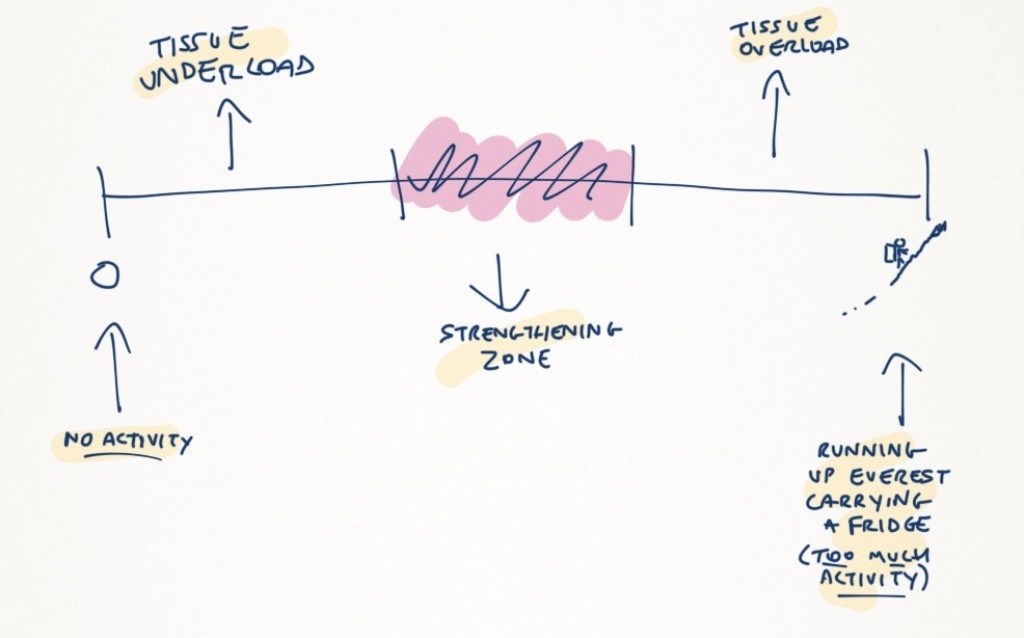
If back pain has reduced your activity levels it’s likely you will have some deconditioning. This means you may have weaker muscles, stiffer joints, decreased flexibility and reduced cardiovascular fitness. The exercises discussed in rehab basics will help to recondition these areas, in doing so making you stronger until you’re able to start running again (or increase your distance if you’re already running). Exercises are best done using pacing too. Too much and you’ll flare up your pain, too little and nothing will change!
Key point: exercise will help strengthen your back which is likely to be deconditioned, use a paced approach doing as much as comfortable and gradually increasing. This is often more helpful than using specific repetitions or sets.
Inactivity can cause as much pain as activity
This is something that affects the spine more than the limbs – staying still in prolonged postures often causes more pain than activity. Two of the most common aggravating factors for back pain are sitting and standing. So pace your sitting and standing. Change position regularly before it starts to hurt. Think about the principles above – find a baseline (how long you can sit/stand for without pain), try and modify – change your sitting posture, try a different chair, use a rolled-up towel to support your back, try a different standing posture or move your legs a little to find a more comfortable position. People ask “what is good posture?” good posture is dynamic posture. Take any opportunity to move. Your body will thank you for it! We see far more office workers with back pain than we see people with active jobs, even those that involve heavy lifting.
For more information on managing ongoing pain see this wonderful website from @paintoolkit2. It’s an excellent resource produced by experts in pain.
Closing thoughts: whether you’re reading this with a niggle or a very painful back pacing and gradual increase in exercise can be the cornerstone of recovery from back pain. It isn’t an easy process and life doesn’t always come in bite-sized pieces that are easy to manage. Even if you can just pace 1 or 2 things it can make a huge difference. If you need help with this process don’t hesitate to ask your GP, Physio or health professional.












Really great write-up (and illustrations). It’s helpful to have a clear picture of what’s going on behind the scenes. I’ve been through this before with several injuries that lingered on for longer than they should have. It’s hard accepting that at least initially you have to scale back on you’re activity, so part of why we continue to push might be denial.
How well do you think the pacing concept works for chronic pain issues outside of the back?
Hi James,
Thanks for your comments. I think pacing works for most things, chronic and acute and not just for backs. It’s about finding the right level of exercise that helps stimulate healing without overloading tissues. So many injuries involve overuse, especially with sport, pacing helps prevent this.
I always had back problems after long runs and my physio discussed these concepts with me and it has worked great. Pacing has really helped me returnto my running, especially after a flare up.
Excellent, insightful article.
[…] – this is such a vital topic that we have a specific article on pacing and pain. In a nutshell it means doing as much as you can manage without increasing your pain. For example […]
[…] Back pain and pacing […]
Brilliant piece of work…..pacing work will definitely increase the capacity of an athlete …
I started getting trouble with my sattaic nerve in my back around two months after running my 1st marathon . After getting an MRI scan done the trouble is what they call a bugle disc trapping the nerve . Could this have cause by doing the marathon .
Tom , geat article , really nice to read and very relevant .
Thanks again
Uzo
Comments are closed.