I was absolutely thrilled when Tom asked me to write this blog on metatarsalgia, a diagnosis I rate right up there with “headache”.
Imagine the scenario, you have consulted eminent Harley Street Physician Sir Rothbart Dingleberry, and describe your symptoms: “Sir Rothbart, I have an aching head”. “I see” his eminence pontificates.. ‘the diagnosis is clear, you have headache. That will be 70 pounds please.”
So it is with metatarsagia, a diagnosis that fairly makes me froth at the mouth when I hear it has been dispensed on an unsuspecting patient.
So.. what IS metatarsalgia? Well, Wikipaedia, as it so often does, has nailed the description thus: “Metatarsalgia (literally metatarsal pain, colloquially known as stone bruise) is a general term used to refer to any painful foot condition affecting the metatarsal region of the foot.”

Bravo, I could not have said it better myself. Like “headache” metatarsalgia is NOT a diagnosis, and in my view is traditionally used by those who either have no idea what the diagnosis is, or are too lazy to go looking!
So, given this understanding, what might metatarsalgia represent? The list is long and varied, and off the top of my head, might include the following actual diagnoses:
1. Interdigital neuroma
2. Metatarsophalangeal joint capsulitis
3. Plantar plate disruption
4. Metatarsal stress fracture
5. Reiter’s Disease
6. Rheumatoid arthritis
7. Tumour
8. Psoriatic arthritis
9. Interdigital bursitis
Now I have deliberately avoided mention of pathology around the 1st metatarsophalangeal joint, because that is another whole can of worms (but in reality would make up the rich fabric of “metatarsalgia”), and one can see that the list above is extremely varied in aetiology, pathology and, ultimately, treatment. And yet, they all are.. metatarsalgia.
For the sake of this discussion, we need to make a few definitions, and delve a little deeper into the complexities of the forefoot, or, as Sigmund Freud put it, “anatomy is destiny” (Freud,S., Collected Writings 1924).
It has been established that by the time an individual reaches 30 years of age, they will have taken in excess of 60 million steps in course of their normal daily activities. This does not include any activities outside those associated with day-to-day living, for example sporting endeavors. Without question, the foot is remarkable. It is the structure responsible for the initiation and execution of that characteristic that sets humans apart from every other species on earth: Bipedal upright locomotion.
The foot is the platform from which, through the coupling mechanisms of the joints, all structures proximally must be dependent. As an exercise in engineering, it is without peer in terms of function, integration and complexity. It is this very complexity that limits our absolute understanding of its mechanical functioning.
We do however now understand that the foot is responsible for much more than just allowing forward propulsion. The sensitive nerve endings and proprioceptors in the foot feed afferent signals to the brain that control many of the delicate adjustments at any level required for effective gait. The brain is constantly monitoring the harmonics of the vibrations caused by impact and forward progression. Many researchers currently believe interference with the frequencies of these vibrations play a key role in injury, because they “scramble” the normal or “correct” message the brain expects to receive. In this instance, it is proposed that injury can occur secondary to altered muscle firing and therefore abnormal loading patterns.
In sport, it is often quoted that impact forces on the foot during running approach three to four times body weight . In addition, the average runner will strike the ground 480 to 1,200 times per kilometre . Whilst these figures reflect a significant load on the foot, its engineering is such that it should easily be able to withstand such load. It is becoming increasingly clear that injury is not precipitated by the load as such, but rather by a caveat to the load, in terms of altered mechanical axes, altered muscle function or changed psychophysical or physiological status.
The forefoot is classically defined as those structures distal to Lis Francs joint, and includes the metatarsals and the phalanges. Whilst the foot can be regionalised, it cannot be compartmentalised, since each region has an intimate and interdependent relationship with the other. The forefoot is primarily responsible for executing the propulsive phase of gait, and, as such, it is required to control the body’s forward progression in a sustained and balanced manner for in excess of 40% of the stance phase of gait.

The forefoot comprises five metatarsals and fourteen phalanges, as well as the associated joints, ligaments and muscles. The metatarsophalangeal (MPJ or MTP), proximal interphalangeal (PIPJ), and distal interphalangeal joints (DIPJ) are condyloid and hinge joints and have a close-packed position in full extension. In addition, the 1st metatarsophalangeal joint has two sesamoid bones insinuated in the tendon of flexor hallucis brevis. These sesamoids function as anatomical pulleys to the flexor hallucis brevis muscle, as well as protecting the tendon of flexor hallucis longus from trauma as it passes between the metatarsal head and the base of the proximal phalanx.
The 1st metatarsophalangeal joint therefore comprises the articular facets of four bones within a single synovial joint capsule. The 1st metatarsophalangeal joint has motion available in two planes, sagittal and tranverse, because of its condylar nature. The motion of the 1st metatarsophalangeal joint is therefore more complex than it may appear, with some authors describing the joint as a “dynamic acetabulum”.
The joint is stabilized medially and laterally by the combined strengths of the collateral ligaments, the suspending sesamoid ligament, and the plantar sesamoid ligament. Further stability is provided by a strong plantar band of tissue comprising the deep transverse metatarsal ligament and associated tissues which prevents separation of the joints under weight-bearing stress.
The forefoot is highly adapted to the enormous shear loads it must accept during running and walking. These forces are especially evident in sport, with stopping and direction changes. The forefoot therefore contains structures which protect against these sheer forces, and concomitantly protect the delicate nerves, vessels and tendons.
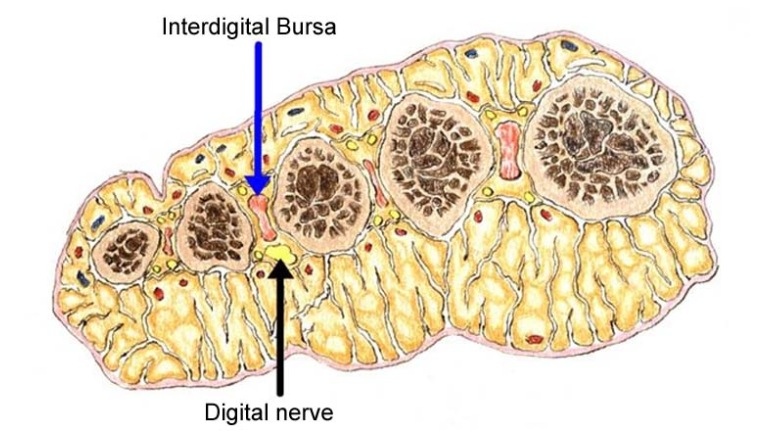
The encapsulated fat pads found in the forefoot and heel have a dynamic protective function superior to anything created in the laboratory. Many athletic footwear companies have attempted to reproduce these properties of human fat pad tissue, and to date have not succeeded.
This image demonstrates the large protective forefoot fat pad, as well as the interdigital bursae and digital nerve, ALL of which might be involved in ‘metatarsalgia”.
The protective properties of this tissue are determined by its unique and ingenious framework of fatty tissue contained within tough bands of tissue running in vertical, tranverse and sagittal directions.
There is a slow degeneration in the plantar fat pad in terms of its size and the quality of collagen, with advancing age. This is coupled to a decreasing load through the 1st metatarsophalangeal joint which leaves the lesser metatarsal heads somewhat vulnerable to injury as we grow older. Altered forefoot mechanics and a general tendency towards increase body weight with advancing years may also conspire toward forefoot injury with age.
A recent paper by Menz et al explores this concept further and may be read here.
It may well be that a future discussion revolves around actual forefoot pathology, what causes it and how to treat it, but for now, the take home message for metatarsalgia is: make the diagnosis.
Modern investigation techniques have vastly improved our ability to visualize not only the relevant forefoot structures, but also the loading patterns imparted on these structures. Ultrasound and MRI are particularly useful around the forefoot, and should, coupled with that most under-rated of clinical skills, history taking, allow the diagnosis to be made.
Modern kinetic investigation, in particular pressure testing, is absolutely invaluable in the assessment of abnormal loading patterns that may lead to forefoot pain. There are now many different systems available, some surprisingly affordable and perfectly adaptable to the busy sports medicine practice. The great advantage of many of the pressure analysis systems is that they operate telemetry systems that are particularly suited to analyzing sports tasks, for example cutting, jumping or running maneuvers in the field.

The real benefit of these systems is that when coupled with the physical exam, history and any other investigation, the actual load through the forefoot can be amortized to the clinical findings. Based on this, appropriate treatment, often involving unloading techniques, can be rapidly instituted.
Perhaps the best we can say right now is that metatarsalgia can be assumed to be related to repetitive high-pressure loading under the metatarsal head that causes pain.
The exact nature of this pain, and the tissues involved, will ultimately determine the line of treatment.
And that is why, for the most part, metatarsalgia is not a term I would encourage any clinician to use on a regular basis. As Fox Mulder (The X-files 1993-2002) said, “the truth is out there”. It is our job to find it.










Thank You!
Very Interesting and Informative
Excellent blog metatarsal pain. But as the author stated, abnormal foot motion can lead to many problems outside of the foot.
The foot to brain connection in the maintenance of postural is an area of research becoming increasing more active. It is becoming apparent that gravity driven pronation results in distorted signals being sent to the cerebellum. The cerebellum acts on these distorted signals, resulting in distorted postural patterns.
And distorted posture is directly linked to chronic musculoskeletal pain.
Prof Rothbart
[…] Metatarsalgia – By Simon Bartold […]
Comments are closed.