Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
Unintentionally this series sounds like a collection of bad break-up lines! So far we’ve had it’s not you, it’s me and it’s not me, it’s you, exploring your role and rehab and whether you may need a second opinion. Next up we examine whether a team approach might be needed to get the results you want.
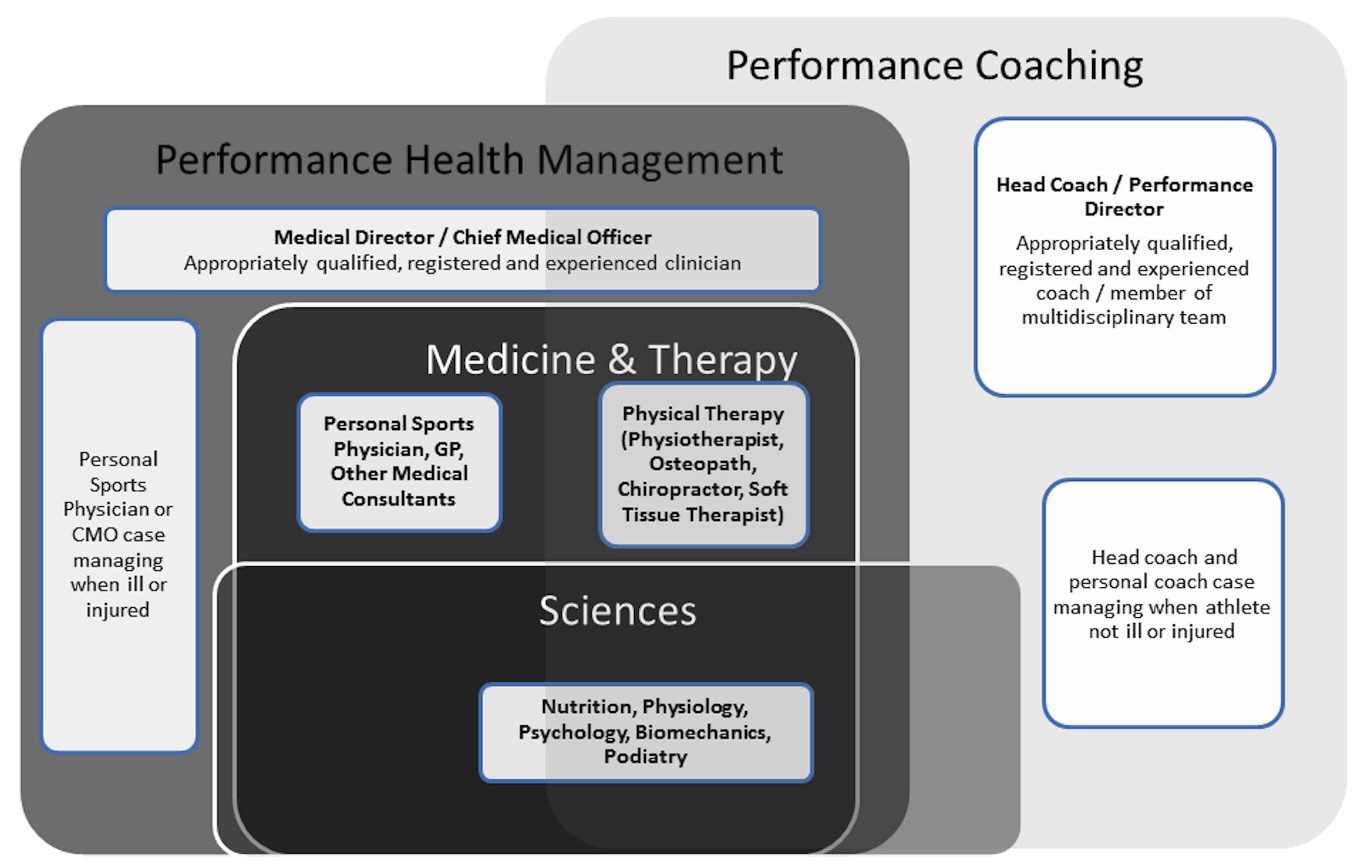
Many running injuries can be treated very successfully by a single therapist without further input from the Multi-Disciplinary Team (MDT). More complex cases, however, may not improve without help from all the right sources.
Let’s use an example of a fictional young female athlete with a suspected bone stress injury to illustrate the importance of integrated care. We’ll call her Alice…
Alice presents with what she describes as ‘shin splints’ – pain up the inside of her shin, along the bone. I’m happy to perform my role as a physio in assessing and treating this injury but part of my role is involving other members of the MDT where indicated.
Referral to a Sports Physician might be indicated to help clarify a diagnosis and arrange further investigation. Specifically, we may want to know if this is a stress reaction or if it has progressed to a stress fracture and where this is located. The physician may also advise on medication, contributing factors and other aspects of treating this injury.
Bone stress injury may occur as a result of training error and an individual’s running gait (e.g. It might be linked to over-striding). Working with a Running Coach to address these areas and plan a structured training programme and appropriate cross-training may be an essential part of the treatment plan.
General health is implicated in bone injury including diet and menstrual function in women. Female endurance athletes may have inadequate energy availability if they are burning more calories than they are consuming. This can have knock-on effects on the menstrual cycle and bone density. Referral to a Dietitian or Sports Nutritionist may be helpful to provide dietary advice. In some cases there may be an eating disorder and input from the psychology team may be required. The patient’s GP will also need to be involved and may assist in returning normal menstrual function.
Input from a podiatrist could also prove hugely useful. Their knowledge of biomechanics, foot function, orthoses and footwear could all help to guide treatment.
Improving muscle strength can help dissipate the load in running to reduce bone stress and may improve performance. While we can provide a rehab programme it may be more effective to work with a Strength and Conditioning Coach.
Alice’s case is just an example and covers just some aspects of the roles of the MDT. It illustrates though that if she only sees a physio vital parts of her treatment might be missing and she is less likely to improve. For example, if Alice’s diet is such that she doesn’t have sufficient energy availability (or enough calcium, vitamin D etc) her bone health may not improve despite physiotherapy.
Source Dijkstra et al. (2014). This open-access article is an excellent overview of integrated care. There is also an accompanying podcast and you can follow @DrPaulDijkstra on Twitter.
Working in a Multi-Disciplinary Team isn’t just a case of having the right team members, it’s essential to work together to provide integrated care to achieve your goals.
We had a recent example of this with tennis pro, Keelan Oakley (@KeelanOakley) who’s kindly agreed to let me talk a little about his case. Keelan had persistent flare-ups of low back pain whenever he tried to return to competition. He had an excellent team behind him including top S&C Coach Brendan Hayes (@theconditioning) and Barry Fulcher (@BF_Tentrade) who’s one of the best tennis coaches in the South. Things really started improving for Keelan when we got together and worked as a team towards key goals, with each of us knowing our roles and responsibilities. He is now back in competition and feeling good!
There are a few practicalities to consider with MDT working;
- Ask your physio or health professional if integrated care is needed and who will make up your team
- Appoint a lead clinician to organise meetings, drive the process forward and make final decisions
- Set an agenda and agree on the aims of MDT meetings to work towards specific goals
- Ensure team members are clear on their roles and responsibilities
- Choose a location where everyone can meet and where practical parts of the process can be carried out if needed. For example, in Keelan’s case, we spent time on the tennis court to review his technique.
- Enquire about cost implications for you
Every situation varies somewhat, with some clinics you may be working with teams that often work together, in others the MDT meeting might be the first time they’ve met! For clinicians, MDT working is a great opportunity to build a network of fellow health professionals and learn from the knowledge and experience.
If you feel you might benefit from an MDT approach you ask your physio/ health professional if it’s likely to help and if they can arrange things for you. It’s very important that the team works together to achieve your goals which leads to our next part in this series…
“We want different things”