Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
Gluteal tendinopathy is a common and frequently disabling condition. Research suggest it affects 1 in 4 women over 50 and has similar effects on quality of life as severe hip arthritis. Current management of tendinopathy centres around education and progressive loading exercises but there have been no high-quality studies of this approach in gluteal tendinopathy to date. That is until now…
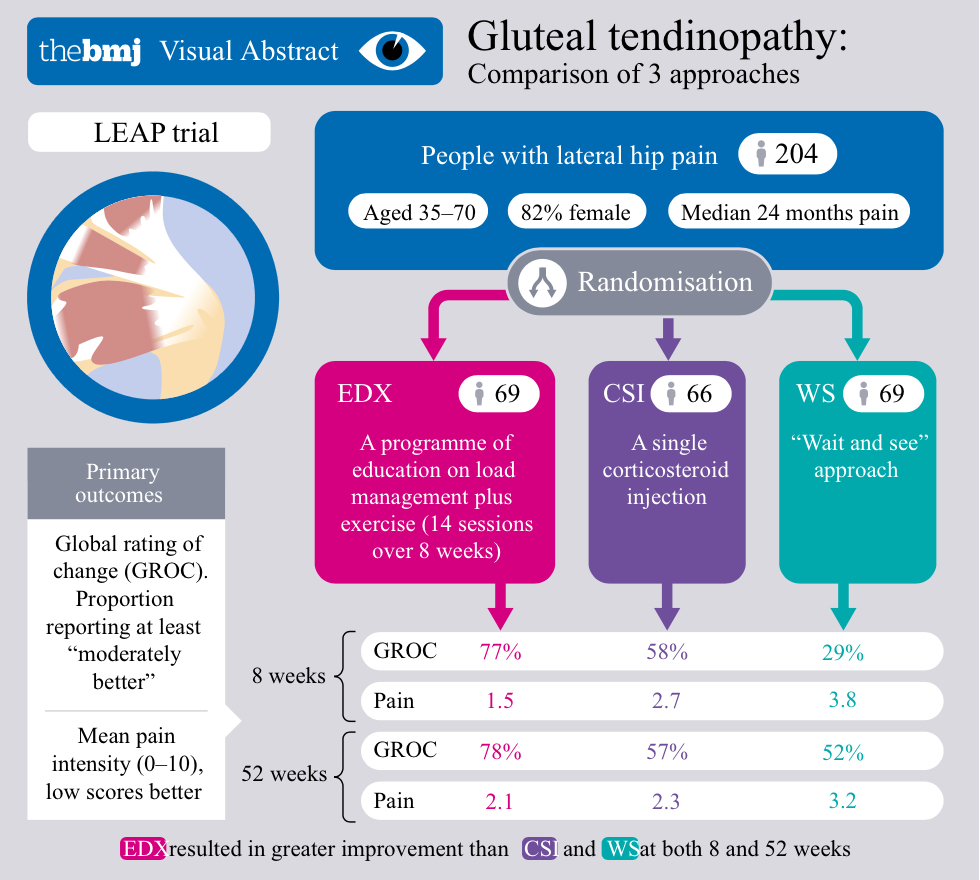
…The prestigious British Medical Journal has just published the LEAP trial, Mellor et al. (2018) which looks set to be a game changer in gluteal tendinopathy (GT)! The study compared education and exercise with corticosteroid injection (CSI) and a ‘wait and see’ group. Participants aged 35 to 70 were included who had lateral hip pain for more than three months with a pain score of at least 4 out of 10 and a clinical diagnosis of GT was reached using a combination of clinical testing and MRI results. In total 204 subjects were studied, 167 of which were women and the mean age was 54.8 years.
The education plus exercise group had 14 physiotherapy sessions over an 8 week period with a progressive rehab programme to improve the load capacity of the gluteal musculotendinous unit and education that centred around avoiding painful compressive movements (such as hip adduction, sleeping and sitting positions). Full details of this approach can be found in the open access study protocol – Mellor et al. (2016), and also within the supplementary material which is excellent! Thanks to top physio Benoy Mathew for sharing the link to this. We’ve adapted and reproduced the rehab programme below;
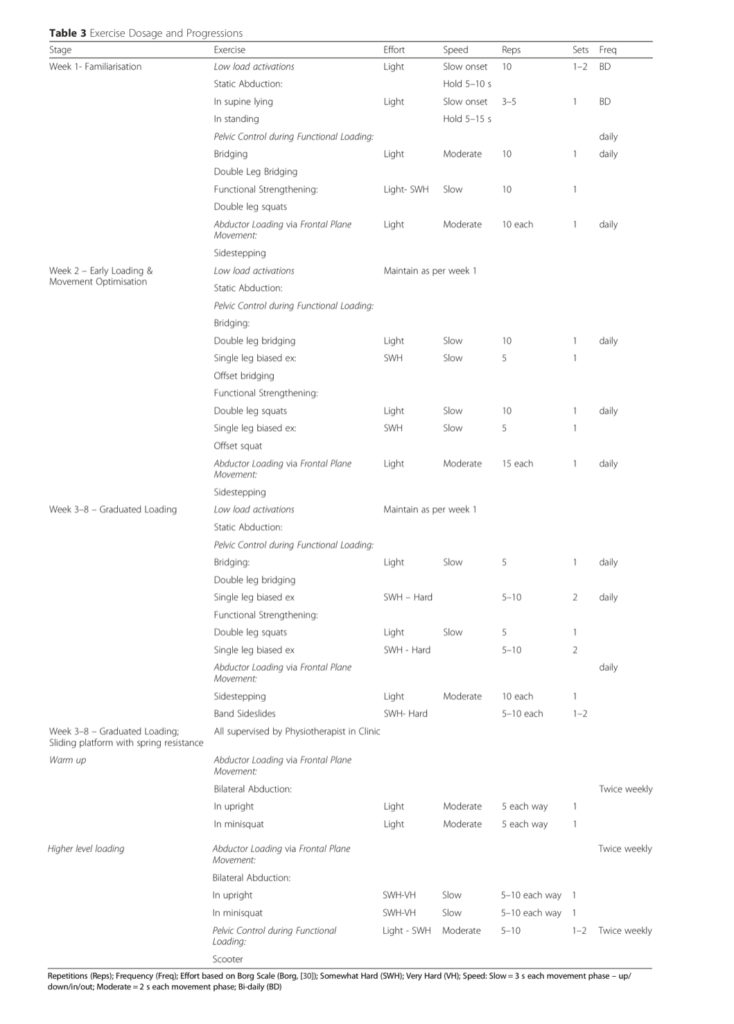
The rehab appears to have similarities with previous tendon studies although there are some notable differences which reflect the needs of this population. It comprised of a mixture of exercises including functional retraining, targeted rehab for the hip and thigh muscles (especially the abductors) and dynamic control of adduction during function. A pain score of up to 5 (out of 10) was allowed during strengthening providing there was no increase in pain that night or the following morning. During ‘functional training’ however no increase in pain was permitted as this was seen as a sign of increased compressive loading.
The difficulty of the exercises was monitored with a Borg Scale and gradually increased providing there was no significant aggravation of symptoms. Like previous work in both patellar and achilles tendinopathy the rehab utilised slow, heavy loading although this appears to have been based on the Borg Scale rather than repetition maximum utilised in other studies (e.g. progressing from 15RM to 6RM over a period of 12 weeks). There is greater variety in exercises than the 3 or 4 used and progressed in Heavy Slow Resistance (HSR) work and it’s worth noting that this is not an eccentric only approach. Taken within the body of evidence this study supports the idea that managing tendinopathy is more abut identifying an individual’s current levels and rehab needs and progressing them towards their goals through individualised rehab than one specific loading approach (e.g. eccentric/ HSR) being applied to all.

Source: Adapted from Cook and Docking (2015) and Cook et al. (2013).
The corticosteroid group had 1 ultrasound guided injection and the waiting list had 1 session with a physiotherapist who provided general information about GT, risk factors, continuing activity and prognosis.
The primary outcome measures in this study were global rating of change in hip condition (an 11 point numerical scale from “very much better” to “very much worse”) and hip pain intensity (the average amount on an 11 point scale from 0 to 10 with no pain at 0 and 10 being worst pain). A number of secondary outcome measures were also studied including the VISA-G questionnaire, patient specific function scale and tests of hip abductor muscle strength.
The results…
Education and exercise performed better than steroid injection and the wait and see approach for gluteal tendinopathy. At the 8 week time point education and exercise achieved an impressive 77.3% success rate on the global rating of change which was superior to both the CSI (58.5%) and wait and see groups (29.4%). Hip pain intensity was also significantly better in the education and exercise group at 8 weeks which would question the common assumption that CSI is superior for pain relief in the short term.
At 52 weeks the global rating of change within the education and exercise group remained significantly better than the other groups with a 78.6% success rate compared to 58.3% and 51.9% for the CSI and wait and see group respectively. At this stage the success rate in the steroid injection groups did not differ significantly from the wait and see approach. It’s interesting to note that over 50% of patients with gluteal tendinopathy in this study had a successful outcome in terms of global rating of change at 1 year without treatment, although both education and exercise and the CSI group reported less pain at this time point. Also of note, although global rating of change was superior in education and exercise versus injection there was no significant difference in pain intensity at 1 year (although both groups remained better than the waiting list).
The graphs below show change in pain intensity and global rating of change over the 52 week period.
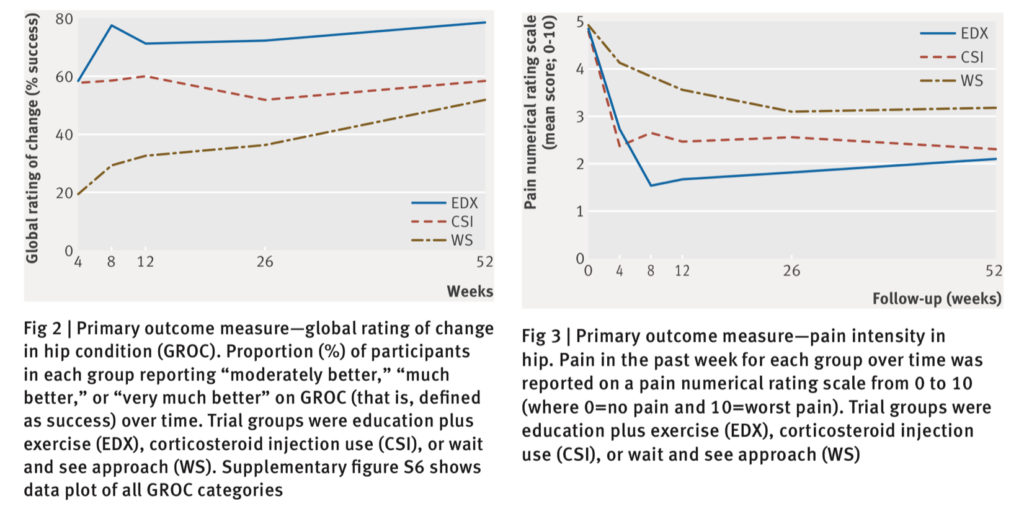
Source: Mellor et al. (2018) OPEN ACCESS.
In secondary outcomes education and exercise again appear superior at 8 weeks,
“Education plus exercise was better than corticosteroid injection use in functional outcomes, quality of life, and self-efficacy measures, and also had less frequent pain and greater clinically important pain reduction” MELLOR ET AL. (2018)
By the 52 week time point the education and exercise group had less frequent pain but there were no other differences in secondary outcomes from the CSI group.
Conclusions
This is the first high quality trial of this kind to show education and exercise can be effective in managing gluteal tendinopathy. The results showed this approach was superior to the wait and see at all time points and outperformed steroid injection, especially at the 8 week stage. By 52 weeks the differences, while remaining significant, have reduced somewhat perhaps indicating regression to the mean for some patients i.e. they simply improve with time.
The paper reveals an intriguing finding that while symptoms differed significantly between the groups at 8 weeks the measures of abductor muscle strength did not. This suggests that it may be the benefits of education rather than increased strength that explain the improvements at this stage. Certainly food for thought and our next article in this gluteal tendinopathy series will explore this in more detail… keep an eye out for that!
My final thoughts on this research is that it’s really encouraging that a body of evidence is developing that supports exercise and education in management of tendinopathy. Such interventions place the patient in control and allow them to progress back towards the activities they love.
For more on management of tendinopathy and running injury register your interest in Running Repairs Online and access our free webinar series on achilles tendon pain or join us on one of our weekend courses.









This post have been extremely informative. I hate the idea of using steroids for anything. They do more harm than good to the body. Also, most of them comes with severe side effects.
You are showing us ways to do away with it. Thank you Tom for sharing this.
I wish they had compared exercise to exercise plus injection (ie what a lot of us do in the real world). Who gives an injection and just leaves it at that?
Comments are closed.