Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
Chronic Plantar Heel Pain (CPHP), plantar fasciitis, jogger’s heel call it what you will persistent heel pain can be a real challenge to treat. It wouldn’t surprise me at all to find out that this condition was the real ‘Achilles’ Heel’ in Greek mythology. I can picture Achilles prostrate on the battlefield, his famous last words, “get me to a podiatrist!…”
…had he been under the care of legendary podiatrist Simon Bartold he’d probably have been fine! Simon is an expert in plantar heel pain so I was delighted when he sent me a brilliantly detailed 2 part blog on the topic. I highly recommend his excellent website, and he’s a definitely one to follow on Twitter via @bartoldbiomechanica. If you like his work, as many do, check out his previous articles for RunningPhysio on “metatarsalgia” and running shoes.
Here’s part 1….
Maybe the most puzzling of all musculoskeletal conditions, plantar fasciitis continues to confound ‘tradtional’ treatment methods, and provide a headache for clinicians. Today, we look at current thought processed on what plantar fasciitis really is, and how to treat it.
Plantar fasciitis is a musculoskeletal disorder primarily affecting the fascial enthesis. It is poorly understood although it is thought to have a mechanical origin.The condition is commonly associated with pes planus and lower limb biomechanical anomalies, with the presumption being that tensile strain on the fascia causes microtears and chronic inflammation. Contrary to clinical doctrine however, the histological evidence does not support this. Inflammation is only rarely observed and scientific support for the role of arch mechanics in the genesis of plantar fasciitis is equivocal. In any case, how does one reliably measure ‘arch mechanics’ in vivo?
With this in mind, it is therefore appropriate to consider what other mechanisms may be involved. Amongst many, we may include:
• ‘Stress shielding’
• Vascular and metabolic disturbances
• Free radical formation
• Hyperthermia
• Genetic factors
All these have been linked to degenerative change in connective tissue.
Let us now turn our attention to what we know.
- Plantar fasciitis is by far the most common sports injury presenting to the sports podiatrist
- With the exception of trauma, it is the most frequent cause of chronic pain in the heel (Riddle et al 2003, Irving, Cook + Menz 2006, Taunton et al, 2002)
- Plantar fasciitis comprises 15% of all adult foot complaints and affects 10% of the population(Rome 1997)
- In the USA, plantar fasciitis accounts for 1 million patient visits per year with the projected cost of $US375 million to third party payers (Tong et al 2010).
However, despite its wide distribution in the sporting and general communities there remains widespread debate on its aetiology. There is also dissatisfaction with a lack of reliable treatment outcomes and the condition is often described as being ‘reliably unreliable’.
There are many treatment options claiming efficacy however, for the vast majority of these interventions, the final outcome varies markedly. The diagnosis of plantar fasciitis is clinical and relies upon a presentation of pain localised over the medial tubercle which is considered pathognomonic and the most widely reported clinical sign. Diagnostic ultrasound demonstrates diffuse or localised hypoechoic areas with thickening. The differential diagnosis for plantar fasciitis is broad, and famous for the inclusion of many descriptive terms amongst specific clinical diagnoses, these including:
• jogger’s heel
• heel spur syndrome
• plantar fascial insertitis
• calcaneal enthesopathy
• subcalcaneal bursitis
• stone bruise
• calcaneal periostitis
• neuritis
• calcaneodynia (DeMaio et al 1993).
In the late 18th century, plantar fasciitis was labelled “gonorrheal heel or lover’s spur” in the belief that all heel pain was a reward for the sins of the flesh!
Let’s have a look at some of the basic anatomy associated with plantar fasciitis.
Gross Anatomy. The plantar fascia is the investing fascia of the sole of the foot and forms a strong mechanical linkage between the calcaneus and the toes. There may be medial, lateral and central bands. Although the medial band is frequently implicated (Kaya1996), in fact it is thin and virtually non-existent at the proximal level (Sarrafian 1987). The lateral band is also quite variable and in some individuals it is fully developed and relatively thick, however, for 12% of the population, it is completely absent. The central aponeurotic band is cited as the major structural and functional component (Wearing 2006) and therefore it is the most likely to be implicated in plantar heel pain.

The plantar fascia is often quoted as a continuation of the triceps surae or plantaris tendon, and this is therefore considered important in terms of aetiology. However Wearing et al (2006) state this is not the case and that the plantar fascia is independent of the tendoachilles in adults. Conversely however, 12% (5/40) of the specimens examined in a study by Kim et al, revealed a partially contiguous relationship between the Achilles tendon and the plantar fascia (Kim et al 2010).
Histological Anatomy. The histological anatomy of the plantar fascia is relatively unknown, however, it is vitally important in understanding the nature of the condition and defining the actual diagnosis. The plantar fascia is a dense connective tissue, likened to both tendon and ligament (Boabighi et al 1993), but with biochemical and histological differences to ligaments of the foot (Davis et al 1996).
So, with this in mind, what exactly is the plantar fascia? It is similar to tendon and ligament, but comprised of elongated fibrocytes embedded in the extracellular matrix consisting primarily of crimped collagen fibres. Fibrocytes produce collagen, and form a 3D communicating network (Benjamin and Ralphs 2000) and it is currently believed this arrangement may be capable of sensing and responding to changes in load. In this way, the plantar fascia may have a great sensory capacity.The plantar fascia also contains more fibroblasts than tendon or ligament. So.. In addition to passively transmitting force, the plantar fascia may act as an active sensory structure capable of modulating its composition in response to external demands. This function is extremely important in relation to understanding the progression and prognosis for the condition, and certainly may influence the approach we take to plantar fasciitis in relation to footwear and orthotic therapy.
The Enthesis. The plantar fascial enthesis is commonly considered the structure involved in plantar fasciitis. Fascia can insert into bone either by direct fibrocartilagenous or indirect periosteal attachment. In the case of the plantar fascia the latter is unlikely so periosteal irritation is an unlikely cause of pain. (Warren 1990) The degree of calcification of the fibrocartilagenous zone reflects the tensile strength of the enthesis and its ability to resist shear, and there is a zone of transition from soft to hard tissue which helps dissipate stress evenly.
Calcified fibrocartilage at the enthesis is more dense than the underlying bone and as such is stiffer, with this being age dependent. This calcification of the entheseal fibrocartilage further increases the brittleness of the enthesis and this may explain the increased incidence of plantar fasciitis in the elderly.
Furthermore, we assume plantar fasciitis is caused by excessive tensile loading at the calcaneal enthesis, however, the histology tells us bending, shear and compression may be at least as important.
Histopathology of the Plantar Fascia. Despite the historical nomenclature of plantar fasciitis, and the direct assumption therefore of inflammatory processes, the histopathology reveals the condition is not primarily inflammatory. For this reason, we shall refer to the condition as chronic plantar heel pain or CPHP from this point forth. It is far more likely the condition may be related to degeneration, this being especially likely since the entheseal tissue in particular, is prone to degeneration.
The histopathological appearance of CPHP resembles the changes seen to articular cartilage during early stage OA with longitudinal fissuring of fibrocartilage, which then ossifies within the enthesis. Spur formation is likely to be a feature. According to McMillan at al (2009), “subcalcaneal spur formation is strongly associated with pain beneath the heel’. A recent meta analysis undertaken by Jill Cook and Craig Purdham (2011) demonstrated that CPHP participants are over 8 times more likely to show evidence of spur than the control group. A recent study by Johal and Milnar (2012) demonstrated that 89% of a symptomatic CPHP cohort had associated calcaneal spur.
In all of this, vertical compressive loading has been identified as more important than traction (Menz et al 2008, Cook and Purdham 2011)
So, the summary so far looks like this:
• The plantar fascia may have significant sensory capacity
• Plantar fasciitis is not primarily inflammatory in nature and therefore should be regarded as fasciopathy with the nomenclature of CPHP (chronic plantar heel pain)
• The enthesis is brittle and therefore susceptible, especially with aging
• Bending, shear and compression are probably more important than tensile load
• The presence of a calcaneal spur is important and strongly linked to CPHP.
With all of this in mind, let’s take a look at who is a risk of developing this pesky condition. CPHP has been reported across a wide sample of the community, including the non-athletic population. It is most frequently seen in the weight bearing occupations, especially factory workers, storemen and nurses. Lutter (1997) reports that 65% of the non sports demographic are overweight, with unilateral involvement most common in 70% of the cases. Most of the literature is in agreement that CPHP occurs most commonly after the fifth decade, and has been attributed to degeneration of the fat pad.
In the athletic population approximately 10% of all running athletes will develop CPHP, with basketball, tennis, football and dance all having noted high frequencies of CPHP, however, long distance running is the activity most often associated with this condition.
There appears to be little correlation between mileage and CPHP, with cases reported from both high and low mileage runners In relation to specific risk factors, a multitude are cited in the literature.
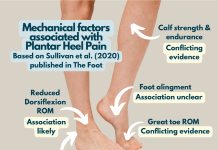
Body mass index (BMI) in a non-athletic population and the presence of a calcaneal spur the two factors found to have an association with plantar fasciitis according to a Cochrane review by Irving (2006). A BMI of 25-30 kg/m2 approximately doubles the occurrence of CPHP, and it triples if passive ankle joint dorsiflexion is less than 10°. It increases by 3.6 times in weight bearing occupations (Sahin et al, 2010).
Obesity and pronated foot posture are associated with plantar fasciitis and may be risk factors for the development of the condition (Irving,D.B., et al, 2007). Wearing et al (2004) looked at arch shape and mechanics and found neither abnormal shape nor movement of the arch are associated with chronic plantar fasciitis, however, arch mechanics may influence the severity of plantar fasciitis, once the condition is present.
The risk factors summary is therefore as follows:
- Increased weight in a non athletic population
- increased age
- decreased ankle dorsiflexion
- decreased first metatarsophalangeal joint extension
- prolonged standing.
All the above have demonstrated some evidence of an association with CPHP (Irvine et al 2006). In part 2 of this discussion, we will examine what evidence exists for many forms of treatment spruiked for plantar heel pain! I will include all references for parts 1 and 2 of this blog in my next posting.








Please inbox me Part 2 – have had this condition for the best part of the last year ..61 years, female, ex-dancer, started leading a more sedentary lifestyle due to depression, cold, inadequate footwear and now can hardly walk normally anymore!! very sore and disappointed, thanks for info so far ( forwarded to me by a caring friend)
Thank you –
pleasure!
Thank You!
Enjoyed Reading, Found The Information Presented Interesting And Informative
Very informative. Acquired this lovely condition following a run on hills. Took month off, ran a shorter 4 mile race and was fine. Soon as I started back to training it returned. I do have the inflammation as well. After fighting the pain and difficulty standing at my job, went to the doc and had an injection. Per his advice, have a new plan. Weaned myself off my inserts, running in low profile shoe, and running only to my heart rate monitor so I don’t over exert myself( 40 min. 3 days a week. Also doing ankle and hip strengthening And stretching. Going on week 3 and so far so good
Please email parts 2 & 3. My daughter has had it for 8mths. Thanks.
Comments are closed.