Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
When something hurts it’s instinctive to want to rub it better, or if possible, have someone else rub it better for you (ooh er missus!). ‘Hands on’ treatment can be an effective part of a treatment plan but rarely, if ever, should it form the entirety of it. Despite this time and time again I see clients who have had no rehab, no training advice just a rub down. So what should form the basis of managing injured athletes?….
I’ve always been a fan of the ‘hands on’ approach. I see it as a useful part of our assessment and treatment process. Recently though I’m becoming increasingly frustrated when I see clients who’ve had no other forms of rehab. Here are some examples;
- Grade 1 calf tear, confirmed with MRI. Still not returned to running 1 year later. Saw three different therapists, given lots of massage and ultrasound but no strength work at all!
- 2 year history of achilles tendinopathy had massage of calf & quads plus hip mobilisation. No rehab exercises or training advice!
- Chronic, Proximal hamstring tendinopathy given 6 session of massage but no rehab or training advice.
Not suprisingly in all 3 cases the athletes had made minimal progress. Whenever they tried to return to running they aggravated their pain and returned to their therapist…for more massage!
I’m in no way anti-massage and shortly Mike Boyce, my colleague from the Physio Rooms, will be discussing the role of massage in a guest blog for us. This isn’t just about massage either but all ‘hands on’ treatments – manipulation, mobilisation, ultrasound, electrotherapy, acupuncture, taping and anything else you can think of! These are all adjuncts to treatment. They assist the core treatments that aim to provide a long term solution by addressing the factors that cause the symptoms;
There are some who may be even more strict than me on this point and suggest these adjuncts have very little research to prove their effectiveness. Their model of care looks more like this;
I include adjuncts mainly because they appear to be effective in reducing pain and assisting rehab. It’s fair to say the evidence to support this isn’t strong in some cases. In general though, research suggests exercise plus hands on treatment is more effective than exercises alone. It’s also fair to say though that in many, many areas in sports medicine there is very little guidance from the literature and a pragamatic approach is required. This involves working with what we find works in practice while integrating what information we do have from the literature.
One thing that appears to unite these treatment adjuncts is we don’t know exactly how they work. While evidence often shows a treatment effect we don’t always know the mechanism of action. As physios and researchers we can get rather hung up on this! It is important of course, but I wonder how important it is to our patients? Are they really concerned if pain relief comes because of ‘breakdown of scar tissue’ (highly unlikely) or from the nervous system’s response to complex touch (more likely)? Or even from placebo (equally likely). The big issue here though is whatever mechanism by which hands on treatments work it’s likely to be fairly short lasting, and unlikely to address the underyling cause. Even more reasons not to rely on hands on treatment on its own.
One point here for therapists – how you describe your treatments is important. You are not ‘putting things back into alingment’ or ‘back in place’. These words suggest to people that joints just slip out of place, they don’t! Our words can cause pain, something described as the ‘nocebo effect’ (demonstrated eloquently in this video).
Athletes, if you’re being told you’re ‘out of aligment’ and need to regularly be ‘put back in place’ I strongly advise a second opinion!
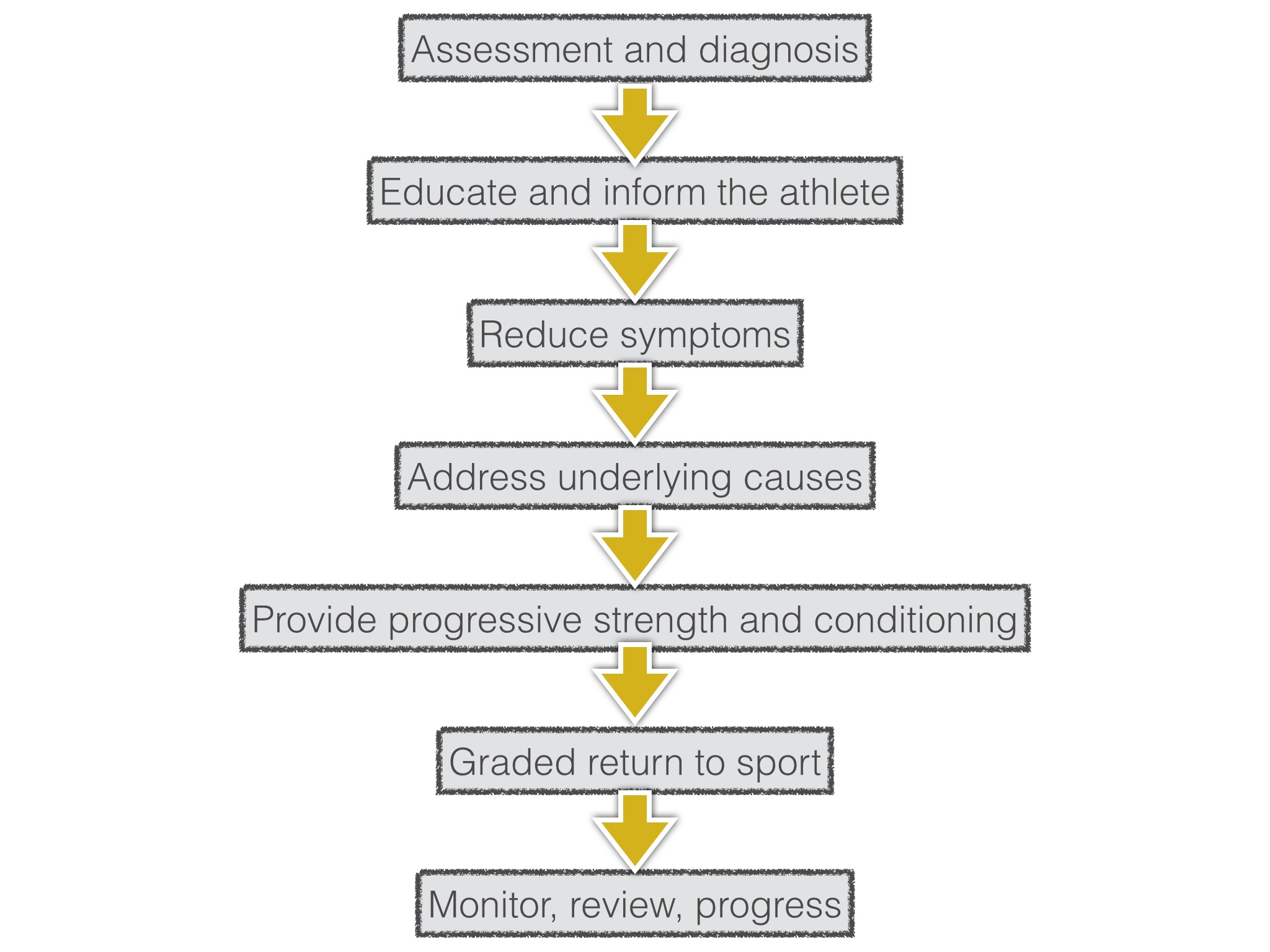
Coming back to my point, hands on may be valuable in reducing symptoms but the effects can be short lived and we aren’t sure exactly how they work – always combine them with a comprehensive rehab plan. Here are some examples of core treatments in common sports injuries;
The table above is by no means comprehensive, and I’m sure some of those ‘core treatments’ may be debateable. What you’ll see is a great deal of overlap between conditions in terms of core principles of rehab. They all have a similar rough overall plan;
The problem is that while our understanding of these conditions is improving, evidence for the effectiveness of specific treatments is still lacking. Jill Cook discussed this in an editorial,
“Evidence-based treatments exist for many sports injuries; for example, reconstruction of the anterior cruciate ligament (ACL) is clinically effective and has evidence to support it. Other injuries that have a more difficult, recurrent or variable time course to recovery, for example, muscle strains, tendon injuries and bone stress, have more limited evidence.”
Interesting that even ACL reconstruction which Jill provides as an example of an evidence based treatment is now being questioned in the literature! Looking at some of the most common running injuries we see a general lack of high quality evidence to guide us;
“Although several investigations have been published, there is a paucity of research of adequate quality on the management of ITBS in runners” van der Worp et al. (2012) – Systematic Review
“At the moment there is limited evidence upon which to base clinical practice” Crawford and Thompson (2003) Systematic Review (updated in 2010 but withdrawn due to lack of new evidence!)
Systematic review by Malliaras et al. (2013) found just 2 high quality studies and identified “paucity of good quality evidence”.
Patellofemoral pain (Runner’s Knee)
Growing body of evidence but outcomes of treatment can still be poor with high numbers reporting chronic or recurrent pain,
“While physiotherapy interventions for PFP have proven effective compared with sham treatments, treatment results can be disappointing in a proportion of patients” Witvrouv et al. (2014)
Medial Tibial Stress Syndrome (‘shin splints‘)
“None of the studies are sufficiently free from methodological bias to recommend any of the treatments investigated” Winters et al. (2013) – Systematic Review
The point I’m making here then is this we shouldn’t be totally dismissive of things that appear to work in practice but lack evidence as we have very little options with a strong evidence base. Equally we should avoid using these treatments in isolation or crediting them with magic powers that they don’t have! Somewhere there is a balance.
Closing thoughts: hands on treatments including massage can be useful in reducing symptoms of injury but you should always ask yourself what is the underlying cause and how can I address it? In many cases there is a combination of training error and muscle weakness, or lack of movement control. Training should be modified to a level the healing tissue can cope with and strength and conditioning can then be used to address any underlying weakness.













Hi Tom. Been reading your blog for a while. Can you give any advice on Biceps Femoris Tendinopathy? Been suffering with it for 8 months and it seems to be getting worse despite numerous physio sessions Basically was told to do various stretches, didn’t work, had ultrasound therapy (despite NHS website saying little evidence that it works), didn’t work, now being told to stretch again and step up and down a step ten times a day. Quickly losing the will to live. Do you see many people with BFT and does it ever heal fully?
Hi Lee, There is always a reason why someone has biceps femoris tendinopathy and stretches, ultrasound, time off, stepping up and down off a step, strength training, etc. won’t help unless it is directly addressing the reason why you have the pain. I am guessing you have the issue only on one leg? This means you have a disparity in the way your right and left legs are working. This imbalance can usually be seen in your hip/pelvis alignment and movement but also in your femur position, foot position, torso and shoulder position, and even arm position and swing. This is because an imbalance somewhere in your body will cause compensation throughout the rest of your body. If you stand relaxed in front of a mirror, you will most likely see one shoulder lower than the other, one hand may hang more forward or pronated than the other, your chest/shoulders might seem rotated slightly, one patella may point slightly in or out compared to the other, and your feet are probably not parallel with the weight perfectly balanced between them. All these imbalances are part of the problem and any treatment that focuses on one area without addressing them all will not fix the problem long term. Their is one area of dysfunction that is probably the cause and the rest is compensation that has built up over the 8+ months and both the compensation and dysfunction need to be addressed and corrected. Yes people with BFT can and do fully heal and get back to pain free running, but only when the entire body is looked at and addressed. My hope is that by now you are back to pain free running, but if not, find someone who will look at and address your whole body and be able to find, explain, and help you correct the underlying cause of the problem. Best, Matt
Loved the article Tom and the video on the nocebo effect. As a chiropractor I cannot tell you the times I have heard from a patient coming from another chiropractor that their “back is out’, ‘hips are off’, ‘leg length is off’, x rays show ‘degeneration’. . . . . this comes from some PT’s too with ‘scar tissue’, ‘adhesions’, – this leads to fear avoidance belief and is harmful. Proper education is key in so many injuries.
[…] More information here on whether you should run or rest and the importance of treatments that address the underlying cause of you injury. […]
Hi Tom, I completely agree that so many people are given “treatments” or “therapy”or “procedures” that they think are fixing the problem and will get them pain free when really all they have been given is at best something that will help the symptom very temporarily. Poor education is always a problem in these cases, but so is the lack of the patients asking good questions. I encourage everyone to always ask the next question. Questions like this are helpful: What caused the cartilage degeneration? How could running cause the cartilage damage if it’s only in one knee? How do you know if one leg is longer than the other? If you adjusted my back and that corrected my leg length difference, than it was never a leg length difference was it? Why is that muscle always tight? Where do adhesions come from? Why is my gluteus medius weak on one side and not the other? What else could be involved? The What, Why, How questions can really help people uncover whether the medical/healthcare practitioner they are working with really knows what they are doing and is really helping them fix the underlying problem or is just giving their regular sales spiel and doesn’t really know why they hurt or how to fix it.
Comments are closed.