Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
When we talk about achilles tendinopathy the mid-portion of the tendon usually hogs the limelight while insertional tendinopathy gets forgotten. It’s important to differentiate between the two and identify where treatment is similar and where it differs.
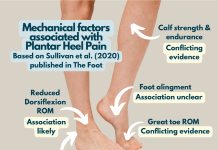
Mid-portion tendinopathy does exactly what it says on the tin – effects the mid portion of the achilles typically 2-7cm above the calcaneus – heel bone (Maayke et al. 2011). The area is likely to be swollen and is often painful when palpated by pinching the tendon. In contrast insertional tendinopathy occurs at the enthesis of the tendon where it attaches to the calcaneus.
A key difference is that compression is considered a key factor in insertional tendinopathy. In the achilles this occurs at end of range dorsiflexion (the upward movement of the ankle). Mid-portion achilles tendinopathy is primarily thought of as a tensile loading problem, rather than compressive, although the plantaris muscle has been considered as a potential source of compression.
Picture source
Our previous article on the staging tendinopathy and role of tendon compression discusses these important concepts more detail. In addition our piece on tendinopathy rehab covers phases of progression. Here we’ll cover the phases on managing pain, building strength and returning to sport.
Phase 1 – reducing pain
Our first priority is reducing pain associated with a reactive tendon. This comprises of three main approaches managing load, isometric exercises and anti-inflammatory medication;
- Managing load – insertional tendinopathy will be aggravated by compressive or tensile loads and with utilising the Stretch-Shortening-Cycle (where the tendon behaves like a complex viscoelastic spring during running, jumping and impact). For the achilles this means reducing activities that involve end of range dorsiflexion (such as walking uphill and ‘heel drops’), tight shoes that cause direct tendon compression and reducing or resting from running. Wearing shoes with a heel may help to reduce load on the tendon while flat running shoes or barefoot style footwear should probably be avoided at this stage. Using a heel raise within your shoe may also help reduce achilles load as a short term measure (Farris et al. 2012). In addition taping techniques that prevent excess dorsiflexion may also be helpful although have very limited research to support their useage. Activities that combine compressive and tensile load should be avoided such as running uphill and stretching the calf muscles. That’s a key point here – dont stretch the calf muscles – it’s likely to aggravate symptoms!
- Isometric exercises – tendon pain is likely to effect muscle function (Henriksen et al. 2011) so using isometric exercises to reduce pain and maintain strength can be very beneficial. The exercise is fairly straight forward – simply push up into a calf raise on both feet and hold for 30-60 seconds, repeat 3-4 times and do 2-3 times per day. You don’t need to push right up on your toes, mid-range is ideal. It’s best to do from the floor, rather than the edge of a step, to prevent ankle dorsiflexion. As pain settles you can progress this to a single leg calf raise.
- Anti-inflammatory medication (NSAIDs) – during the reactive stage of tendinopathy NSAIDs such as ibuprofen can be helpful to reduce tendon swelling and pain. However always consult your GP or pharmacist before taking medications. It’s important to point out that technically the tendon isn’t really inflamed and that long term usage of NSAIDs is not recommended and may even be detrimental to tendon healing. The medication is thought to work in the reactive stage by regulating the activity of tenocytes (cells within the tendon that produce proteins which promote swelling).
Phase 2 – building strength
Once the pain has settled the next aim is to improve the load capacity of the muscle and tendon by improving calf strength. Your Physio should guide you on when to progress your rehab. As a general guide you should be able to manage 10-15 single leg calf raises with minimal increase in your pain. If your symptoms haven’t settled to this extent continue isometric work and discuss it with your Physio.
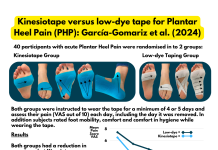
The calf complex is composed of 2 main muscles – gastrocnemius and soleus – both need to be strengthened. The most simple way of achieving this is by doing calf raises from the floor (rather than on the edge of a step). Research on strengthening specific to insertional achilles tendinopathy is sparse. The most promising study appears to be that of Jonsson et al. (2008) who used an eccentric programme with similar approach to Alfredson et al. (1998). There was 1 crucial difference – they avoiding loading into dorsiflexion. They used 1 key exercise doing a calf raise on the good foot then eccentrically lowering to the ground on the injured one (with the leg straight). Patients completed 3 sets of 15 reps twice per day, 7 days per week for 12 weeks and progressed load with a weighted back pack. After this 67% of patients were satisfied with their outcome and had returned to their sport. By contrast Rompe et al. (2008) exercised into dorsiflexion (on the edge of a step as per Alfredson et al. 1998) and just 28% of their patients reported complete recovery or significant improvement.
Source Jonsson et al. (2008) – freely available online here.
Since Jonsson’s study our knowledge in tendinopathy has developed a great deal. Recent work by Malliaras et al. (2013) has shown that we needn’t remove the concentric component of the exercise. The key aim is to improve the ability of the tendon and muscle to manage load which can be achieved through strength training with heavy load.
To achieve this start with single leg calf raises a) with the leg straight and b) with the knee flexed 20-30° to target soleus. Flexing the knee does create some ankle dorsiflexion which can be painful, if so start with the knee flexed just 10-15° and progress when comfortable. Wearing a trainer with a reasonable heel on it or starting the exercise with the heel already an inch or 2 off the floor can also help. The exercise doesn’t involve end of range dorsiflexion so isn’t likely to cause significant tendon compression. That said, Clinical Specialist Richard Norris recommends just doing the eccentric phase (the lowering part) with a book under your heel to prevent excess dorsiflexion.
Your Physio should guide you in terms of reps and sets. As a general rule start with around 3 sets of 15 reps for each exercise, with a 2 minute rest between sets. Repeat this 3 days per week with a rest day between each session. When you can do this with minimal pain try increasing the load using a weighted back pack or holding a heavy dumbell in one hand (while using the other hand for balance). You can also use the Smith Machine in the gym or calf raise on the leg press.
Heavy loading is thought to stimulate the most adaptation from the muscle and tendon. Gradually progress your load to the point where you can only manage around 12 reps with good technique. This is known as 12 rep max (12RM). Aim for 3 sets of 12 reps both the knee straight and flexed (as detailed above).
Monitor your response to loading – some mild pain during exercise is acceptable if it settles quickly and there are no additional morning symptoms the following day. As the exercises become easier increase the load and gradually reduce the reps so you are working at 10RM then 8RM. You may even want to progress to 6RM but be guided by your Physio and your symptoms.
A graded increase in load during exercise in this way follows research from both the ACSM and Kongsgaard et al. (2009 & 2010). The ACSM (2009) recommend working in a range of 8-12RM for improving strength and Kongsgaard et al. used a progressive loading programme (in patellar tendinopathy) which started with 15RM and progressed to 6RM over a period of 12 weeks.
Return to running
Your Physio should guide you on when to return to sport. Ideally you should have equal strength left and right with straight and bent leg calf raise. Use your 10RM as a measure. In addition functional tests, such as repeated hopping on the injured leg, should be pain free.
In Jonsson et al. (2008) patients returned to their sport after 6 weeks of strength training. However it should be noted that they had symptoms for an average of 26 months so it’s less likely they were in a reactive stage (where running is highly likely to aggravate). Silbernagel et al. (2007) included patients with at least a 2 month history of mid-portion achilles tendinopathy, which is perhaps a little more representative of the majority of people with this condition. They allowed returned to sport providing pain remained below 5 out of 10 on the pain scale while exercising and there was no increase in symptoms the following morning. Kongsgaard et al. were a little more cautious in their studies, recommending pain was below 30 out of 100 (so essentially 3 out of 10). The most sensible approach is probably to stick to the ‘safe zone’ of 0-3 out of 10 as it is less likely to aggravate symptoms after and running with 4-5 out of 10 pain is pretty uncomfortable.
In essence the key here is a gradual return to running while monitoring symptoms to prevent excessive reaction. Mild pain when running is acceptable but should settle quickly after. Mileage should be increased gradually and ideally 1-2 rest days should be left between runs to allow the tendon to adapt and recover.
Avoid hill running initially as this will require more ankle dorsiflexion when going uphill and is more likely to lead to tendon compression and aggravate symptoms. In addition running shoes with a larger heel section are probably preferable to flat shoes as they may prevent excess dorsiflexion and reduce load on the achilles.
Limitations and recent research
It’s important to note that there are several limitations of our recommendations that have been highlighted by a recent systematic review. Wiegerinck et al. (2013) found just 4 studies on eccentric exercise for insertional achilles tendinopathy that met their inclusion criteria. In total these papers included just 92 patients in total. When the results of the studies are combined the overall average improvement on a 10 point scale was just 2.7 points and only 42% of patients reported being ‘satisfied’ or ‘extremely satisfied’ with their outcome. However, if the research is divided into studies that exercised into dorsiflexion and not into dorsiflexion the results are quite different. 3 studies work into dorsiflexion and reported just 30% were satisfied with their outcome, while 1 study (Jonsson et al. 2008) avoided dorsiflexion and reported 67% were satisfied. This highlights the importance of strengthening in a way that avoids excess dorsiflexion i.e. not ‘heel drops‘.
No studies included by Wiegerinck et al. in their review examined exercising both concentrically and eccentrically (pushing up and lowering down during a calf raise). It appears our evidence base for deciding loading programmes specifically for insertional achilles tendinopathy is based on a single pilot study involving just 27 patients and a relatively short follow up period.
Our recommendations are based on theoretical research on tendon pathology and function and the use of exercise to treat more common tendinopathies. Even within this the evidence to support specific approaches is limited. Malliaras et al. (2013) reviewed loading programmes and found just 2 high quality studies!
Closing thoughts: insertional achilles tendinopathy can be challenging to treat. Aggravating factors involving loaded dorsiflexion movements need to be reduced at least in the short term. Combining this load management with isometric exercises and NSAIDs will help pain in the reactive stage. Following this strengthening the calf muscles with progressively heavier loads in positions without excess dorsiflexion will improve tendon load capacity and help facilitate return to running. Despite this some cases will require more extensive rehab. What little research there is suggests a large group (at least 33%) don’t completely recover with this approach. In these cases progression through the phases or tendinopathy rehab to include functional strengthening, correction of movement dysfunction, power training, plyometrics to engage the Stretch-Shortening-Cycle and sports specific rehab may be indicated. This should be based on each individual and requires detailed assessment from a physiotherapist or health professional…as ever on RunningPhysio if in doubt get checked out!
And finally…
A big thank you to Peter Thain and James Welch for their help sourcing research for this article.
Peter (@MrThain) has been a great support to the site and wrote us a excellent guest blog on using ice after injury.
James (@Ablefeet) is a top podiatrist and my go to guy for anything feet related. If you live in Surrey and need a podiatrist he’s your man! – http://www.ablefeet.com/












[…] his website. We've teamed up to put together some additional information to compliment our previous article on this […]
Hi,
Currently suffering from an angered achilles and stumbled on your blog whilst searching for help. Wonderful detailed posts, thank you! I’m curious – is it possible to have both mid-portion tendinopathy and insertional tendinopathy at the same time or would the heel pain be indicative of some other accompanying irritation (e.g. plantar fasciitis)? If it is possible to have both, how would you treat since many of the approaches for mid-portion tendinopathy seem to involve exercises that are contraindicated for insertional tendinopathy. (e.g. stretching/rolling out the calf muscles).
Thanks once again, keep up the awesome blog!
Laura.
Hi Laura,
I don’t know if you are still following this blog. I have pain at both mid-portion and insertinal parts of my achilles tendons accompanied by some heel pain. Did you finally get rid of your pain? Did the advice/exercises of this post work?
Will be greatful if anybody can share his/her successful experience here!
Hi
Great article and very interesting about the latest research (Malliaras et al, 2013) illustrating that concentric contractions are not so ill-advised for insertional T.
Have had this over several years now and within the past year this has finally developed to stop me from running. So haven’t run in about 8 months and have been doing eccentric work for about the same time. Started with drops to floor, as per Jonsson et al (2008), but when visited physio she told me to drop into dorsiflexion and add intense finger massage to area. This helped a bit but when I progressed to more dynamic work, the symptoms flared up again and she told me to drop back on the work. Anyway, this hasn’t improved despite my diligence with conservative treatment and I’m seeing the consultant tomorrow for an opinion on an op.
In terms of Laura’s question – when I had my ultrasound they discovered slight tendinopathy in the upper portion of the achilles too although the main problem was the insertion area and calcification. So yes, I think you can have the two ‘types’, as it were, but I think the treatment has to be for insertional initially, which may enable you to progress onto dorsiflexion for the upper portion later on. Otherwise you won’t get past the irritation and pain in the lower, insertional area. Just my view…
Rob
I’ve been suffering from IAT (I think) for almost 1.5 years. It’s been incredibly depressing to realize how little the medical profession knows about tendons and how to alleviate their pathies and osises. and this is the first place I’ve seen a routine articulated that MIGHT allow me to get back to doing anything active outside again. Thanks for this.
Being compliant with PTs has only wasted hours/weeks/months and cost me hundreds of dollars, so goodbye to that. Next week I will shoving this piece in the face of my 4th different physical therapist asking them why we’re not following it (Yes, I’ve seen three separate outfits over the last year for this problem, and my mistrust and skepticism of physical therapists couldn’t be greater than it is now).
They’ll probably try to make me do some ‘core strengthening’ exercises too, which I’ll do but see as irritating busy work more than anything else.
I am suffering from insertional tendinopathy and may be some plantar fasciitis
I agree this problem is very frustrating, I have tried anti inflammatories, ice, heat, acupuncture, wearing a cam boot, sometimes a splint at night, staying away from sports up to 6 weeks.
I also have tried some physical therapy, eccentric stretching and strengthening ( I started to do so but the sports medicine MD told me to hold those exercises for some time)
I still have pain, I do not walk as before, I am limping a little bit
I will see a Doctor, orthopedic surgeon , who deals only with foot and ankle problems, in a large university center, see what’s her opinion. My opinion, knowledge about this issue is rather poor.
Great advice… thanks 🙂 … i’m a sprinter and have been suffering from IAT on and off every time I train for explosiveness.
I will test out these methods over the next 6 weeks but am keen to know if i should progress on to exercises into dorsiflexion after my strength has increased on the 4 exercises below:-
1) double leg isometric exercises 60 seconds x 4 sets 2-3 times a day
2) single leg isometric exercises 60 seconds x 4 sets 2-3 times a day until the pain is gone
3) single leg calf raises with the leg straight 15 reps x 3 sets with 2 min recovery 3 times a week
4) single leg calf raises with the knee flexed 20-30° to target soleus 15 reps x 3 sets with 2 min recovery 3 times a week.
(i’m thinking if I don’t strengthen through the dorsiflexion phase of movement as soon as I start sprinting again I might re-aggravate it):-
Let me know
Thanks
Clare
[…] Insertional achilles tendinopathy: this is when the pain is in the heel not the mid-portion of the […]
An additional treatment option to consider is Platelet Rich Plasma Injections. I have a quite severe case of Achilles tendinopathy due to years of running and running at a high level into my late thirties. I also had a lot of scar tissue in my calve muscles from multiple tears. In any event, in 2007, my running came to a halt and I have been enduring years of physiotherapy that resulted in the scar tissue in my calves being broken down to a certain degree. Last year, I finally started receiving PRP injections as well as trigger point injections into the balled up areas of scar tissue in my calves. If I had received this treatment in 2007, I wouldn’t have ended up with a damaged Achilles tendon and I would still be running. The PRP has decreased the thickness of my Achilles tendon and significantly decreased the pain and I am starting to train my Achilles to function properly with TRX training. I’ll keep you posted on whether I ever run again.
i too am getting prp. how is your pain level now?
Did PRP work ?
Nice to hear from fellow sufferers of this terrible -opathy! Giving an update six months hence…I’ve been able to get back to some running with the help of physical therapist #4 (ran my first 10K on Thanksgiving!). Two things I learned that may be of help to others.
1.) Finding the root cause of the problem is really important (if possible). In my case, a sedentary childhood led to a non-used left glute muscle. Like, I never used it for anything, ever. So the rest of my leg was all out of wack, and in the end problems revealed themselves as IAT, lucky me. Took me several weeks to learn how to activate my left glute, and I’m still working on a) strengthening my left leg, and b.) running form that uses my butt more effectively and won’t give me other problems; last run I had I think my quad tendon was starting to strain a bit, ugh.
2.) Once any chronic -opathy condition sets in, at some point you might have to overcome a chronic pain problem that is independent of the original issue. For months I had ceased exercising whenever my heel/foot started hurting more than a little, for fear that I was making my tendon problems worse. I finally got advice that I should keep exercising/running through some moderate pain, just to see what happened (this was after PT #4 said they couldn’t see any obvious cause of my pain any longer). Miraculously, the next day the pain I had had for over a year went away almost altogether.
So, My IAT had actually gotten better over many months of effort, rest and therapy, but my brain just hadn’t gotten the memo.
I really feel for those with worse tendon damage than mine. My ankle joint is still causing me some trouble, but at least it doesn’t hurt continuously at that g***** insertion point anymore.
The best advice? Finding someone who can help you that knows what they’re talking about. I can’t thank Julie enough after all the months I wasted with other physical therapy outfits.
Hi Jon,
I know this thread is a really old one but wondering if you are still in a good place with this…
Congratulations on your recovery! I would love to be able to tell the same story one day.
I believe my situation is similar to yours (had to activate other muscles, insertional, 15 mos. now). I, too, feel that I am doing the wrong things given the time I’ve taken off of running and the various podiatrist sessions, drops, etc.
I do the very same thing you describe – I feel good, start to jog/light run, feel a bit sore the next day and shut it down for weeks, or months, at a time. It’s a cylce I seem to forget because I start it up again and again with the same result. Was it actual pain while running or just the in-between exercise creakiness/post-exercise (mine) that you eventually had to overcome? I struggle with understanding what is chronic inflammation and what is actual damage.
Your thoughts are appreciated.
Greg
Wonderful article. Thanks. I have Posterior Achilles tendon bursitis pain at the point of insertion with the heel bone(courtesy those tight soccer shoes and their rigid heel counter). I’m considering returning back to running. I’m mostly a heel striker, but some of my friend that are into distance running are suggesting to try mid foot strike for reducing pain. Can you pl. let me know if mid foot strike will make any difference. I got gait analysis done at a nearby specialised running store and it turned out to be that I have normal feet with very minimal pronation on the leg where the surgery was performed
PS : I had tried conventional methods (inserts, NSAIDs, isometric exercises etc.,) and since there was no luck, I had the growth on my left heel removed surgically. I don’t have the guts to do that again on the right heel.
How it was with the surgery you had? Did the heel bone stop hurting your aquiles tendon?
Comments are closed.