Our articles are not designed to replace medical advice. If you have an injury we recommend seeing a qualified health professional. To book an appointment with Tom Goom (AKA ‘The Running Physio’) visit our clinic page. We offer both in-person assessments and online consultations.
Dr Christian Barton is a multi-published researcher with a very successful clinic and excellent blog. He is one of the leading names in patellofemoral research and so I was delighted when he agreed to write for RunningPhysio. He is currently working on running gait re-training research and runs a number of courses which I highly recommend to fellow physios. Today he’ll be covering hip strength and patellofemoral pain. Follow Chris on Twitter via @DrChrisBarton.
In recent times, significant attention has been paid to the relationship between hip function and patellofemoral pain (PFP).[1] Chris Powers published a very nice theoretical paper on this in 2010 titled ‘The influence of abnormal hip mechanics on knee injury: a biomechanical perspective.’ This is well worth reading if you haven’t done so already. Put simply, excessive femoral internal rotation and adduction is thought to lead to lateral patellar tracking, and subsequently increased lateral patellofemoral joint (PFJ) stress. When describing this concept to patients, I like to use the term “the tracks moving underneath the train.” Importantly, previous work by Rich Souza and Chris Powers has indicated that during weight-bearing activity, this is exactly what leads to lateral patellar tracking – i.e. the femur rolls under the patellar.[2] Contrary to this, in non-weight-bearing, it is the opposite, with “the train moving off the tracks” – i.e. the patellar tracks laterally relative to the femur. These findings further highlight the need to shift focus away from VMO retraining, and think more about the rest of the kinetic chain, in particular the hip.
Figure 1 A = Lateral patellar tracking during non-weight-bearing quadriceps contraction (train moving on tracks); B = femur medially rotating under patellar during weight-bearing quadriceps contraction (tracks moving under train). Image taken from Souza and Powers.[2]
Recent prospective research has provided support to the importance of the hip in patellofemoral aetiology. Specifically, increased femoral internal rotation during jump landing in military recruits,[3] and increased hip adduction in female recreational runners[4] have both been reported to be risk factors for patellofemoral pain development. It is highly plausible that these biomechanical deficiencies are the result of impaired hip (gluteal) muscle function. In fact many recent PFP rehabilitation programs in research and clinical practice have focussed on strengthening the hip musculature, with the belief that weakness exists, and addressing it will lead to better hip control.
We recently completed a systematic review and meta-analysis, led by Michael Rathleff, to explore the relationship between hip muscle strength and PFP. Further details regarding methodology and the full review can be found in the subsequent British Journal of Sports Medicine publication.
What we found
- Based on data pooling, it is clear that adults with PFP have isometric hip strength deficits
- Greater isometric strength deficits exist in females with PFP, compared to males
- Adolescents do not appear to possess the same strength deficits as adults
- There is a discrepancy between prospective and cross sectional findings, with data pooling from a small number of studies indicating, hip strength may not be a risk factor for PFP development
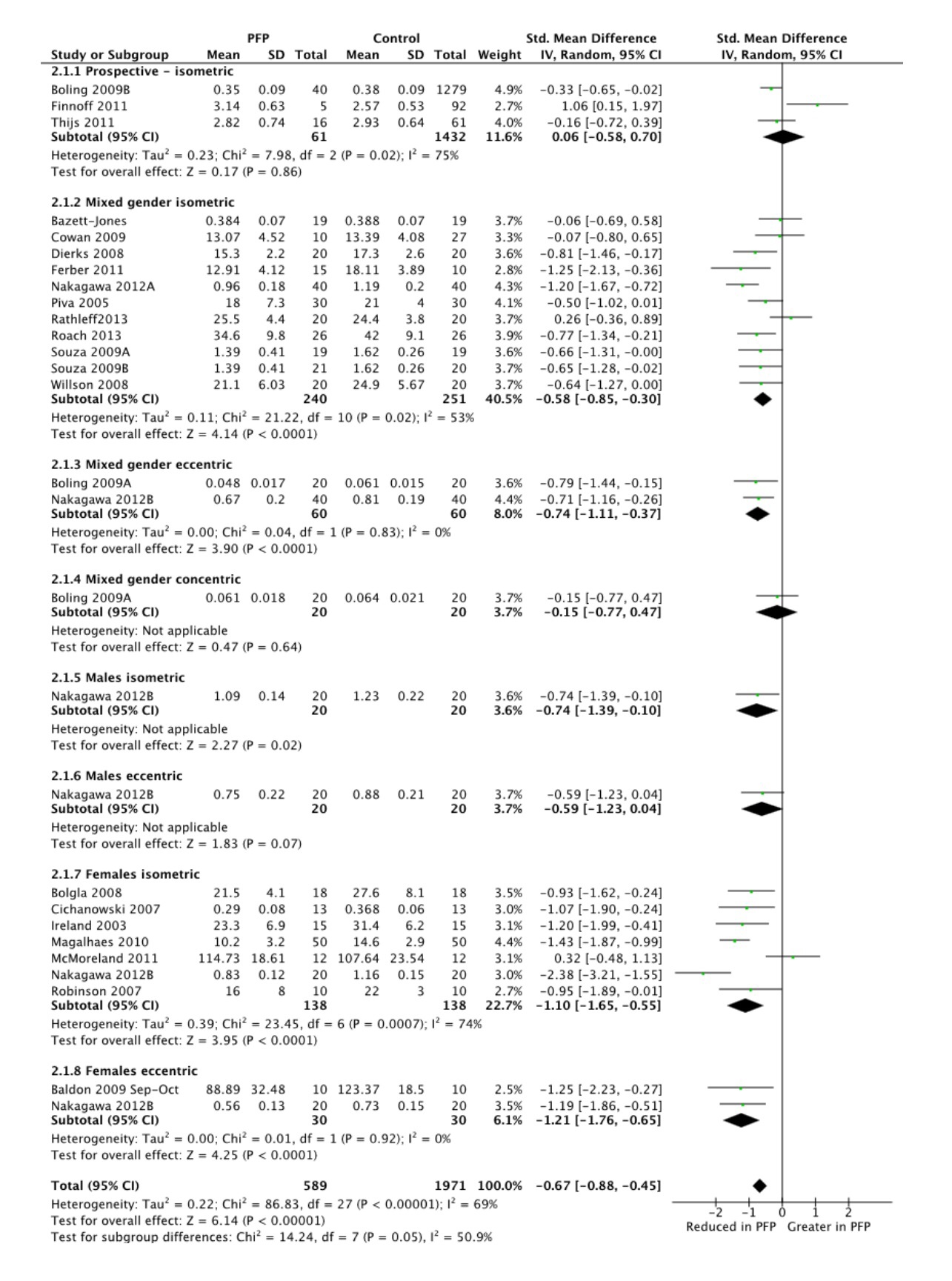
Figure 2 Isometric hip abduction strength in individuals with and without PFP. Further figures available in publication
Clinical implications
Hip weakness is likely in adult patients presenting with PFP, especially females. Additionally, there is clearly growing evidence to support the efficacy of hip strengthening in the management of PFP.[5] Therefore, it is difficult to argue against the importance of including hip strengthening exercises during the rehabilitation of patients with PFP.
Interestingly however, there is a discord between prospective and cross sectional findings, with currently limited research indicating hip strength is not a risk factor for PFP. There appears to be a poor association between hip strength deficits and adolescent PFP, indicating hip weakness may be the result of long standing PFP rather than a causative factor. An additional important finding in this review was that hip strengthening in individuals with PFP does not seem to alter knee or hip motion linked to increased risk of PFP development,[54, 55] indicating the likely need for concurrent movement pattern retraining. Nonetheless, the strengthening programs did effectively reduce running related pain, possibly as a result of reduced knee joint moments and improved shock attenuation (Nb: further research is needed to explore this).
Conclusion
Hip strength deficits exist in individuals with PFP, and more so in females. Although addressing hip strength deficits is an important component of rehabilitation in PFP management, it is only one piece in the puzzle. We know that PFP is a multifactorial condition, with consideration of a range of local, proximal and distal factors needed. Most importantly, when addressing hip muscle function, focussing solely on strength may not be the most effective strategy. Addressing hip strength deficits is important, but consideration to other strategies such as neuromotor and gait retraining is needed to address other known hip related risk factors such as increased hip adduction and internal rotation. Addressing hip strength alone is unlikely to get the job done.
References
1. Powers, C.M., The influence of abnormal hip mechanics on knee injury: a biomechanical perspective. J Orthop Sports Phys Ther, 2010. 40(2): p. 42-51.
2. Souza, R.B., et al., Femur rotation and patellofemoral joint kinematics: a weight-bearing magnetic resonance imaging analysis. J Orthop Sports Phys Ther, 2010. 40(5): p. 277-85.
3. Boling, M.C., et al., A prospective investigation of biomechanical risk factors for patellofemoral pain syndrome: the Joint Undertaking to Monitor and Prevent ACL Injury (JUMP-ACL) cohort. Am J Sports Med, 2009. 37(11): p. 2108-16.
4. Noehren, B., J. Hamill, and I. Davis, Prospective evidence for a hip etiology in patellofemoral pain. Med Sci Sports Exerc, 2013. 45(6): p. 1120-4.
5. Peters, J.S. and N.L. Tyson, Proximal exercises are effective in treating patellofemoral pain syndrome: a systematic review. Int J Sports Phys Ther, 2013. 8(5): p. 689-700.











[…] “Is hip strength a risk factor for patellofemoral pain?“, by Christian Barton, PT, PhD […]
Hi,
Another really good, well balanced article – Thanks for posting. I wondered what gait retraining cues you use to compliment the hip strengthening. The main areas I look at are 1) step width if they have a cross over gait – my reasoning to decrease any valgus moments and potentially place the femur in a better position for glutes to fire 2) An increase in cadence (if its low) – my reasoning being to decrease ground contact time and therefore decrease the time and range of hip drop/knee valgus/IR.
Any thoughts? i’d appreciate your expertise.
Hi Christian, Thanks for the good common sense article. The best therapists in the world are always asking more questions and never assuming they have it already figured out – you are obviously in that category! Have you looked at the relationship of psoas and iliacus weakness in PFP? I have found many times there are unaddressed imbalances in those muscles and weakness can contribute to excessive internal femur rotation and valgus knee stress. The other factor I have found missed by many therapists is the involvement of upper body postural imbalances – specifically torso rotation – that cause compensatory and dysfunctional movement patterns in the lower body. Without addressing the upper body imbalances, the lower body will not permanently change its movement patterns. I would love to hear your thoughts and experience. – Matt
[…] Is hip strength a risk factor for patellofemoral pain? – By Dr Christian Barton […]
Since I begun moving to gluteal and core strengthening for patellofemoral pain I have been getting much better outcomes. VMO strengthening is annoying to say the least and I have yet to find an exercise that is effective in isolating the VMO reliably. Good to see that my change in practice was based on more than a hunch.
[…] Is Hip Strength a Risk Factor for Patellofemoral Pain? […]
[…] Is hip strength a risk factor for patellofemoral pain? – By Dr Christian Barton Should I stop running? […]
Comments are closed.